About Dr. Asheesh Tewari

Dr. Tewari is a surgeon specializing in the diseases of the retina, vitreous, and macula. Born and raised in Detroit, Dr. Tewari graduated with honors from Wayne State University School of Medicine. He then completed his ophthalmology residency at the Kresge Eye Institute, where he served as Co-Chief Resident. He completed a vitreoretinal surgery fellowship at the Barnes Retina Institute located at Barnes-Jewish Hospital/Washington University in St. Louis, Missouri.
He served as an Associate Professor in the Department of Ophthalmology at Wayne State University Medical School and the Kresge Eye Institute. In addition, he was the Director of the Vitreoretinal surgery fellowship. He is also founder of the Michigan Retina Center, a clinical practice with offices in Dearborn and Ann Arbor. He has written numerous articles and chapters for publication in national and international publications. He has also been a speaker at many ophthalmology lectures and meetings. His interests include diabetic eye disease, macular degeneration, surgical treatment of diabetic retinopathy, and complex retinal detachments. His recent work has focused on new surgical techniques, including small gauge vitrectomy and instrument design. Dr. Tewari is an experienced surgeon who treats vitreoretinal conditions using the latest surgical techniques. He was among the first surgeons to employ 23-gauge vitrectomy for the repair of vitreoretinal diseases. Dr. Tewari stays on the leading edge of innovative surgical techniques. He is board certified by the American Board of Ophthalmology.
Transcription of the interview
Asheesh Tewari (00:14):
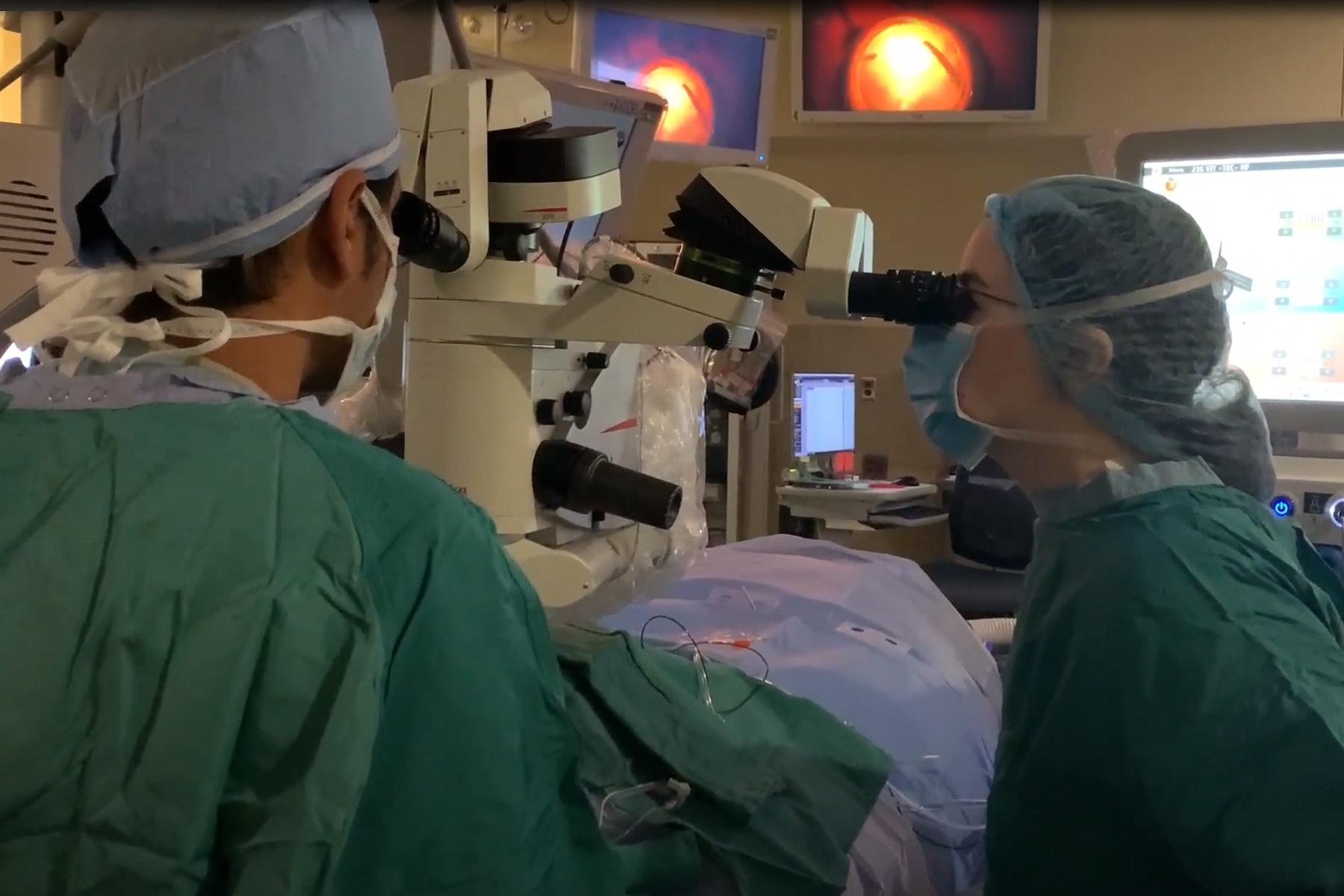
My name is Dr. Asheesh Tewari and I'm a retina specialist at the Michigan Retina Center. We are a practice that's focused on the medical and surgical diseases of retina and we're based in Ann Arbor and Metro Detroit. Prior to this, I was on faculty at the Kresge Eye Institute at Wayne State University for over a decade and was involved in the training of our retina fellows. We do our surgeries at St. Joseph's Hospital in Ann Arbor and use the Proveo microscope exclusively.
Asheesh Tewari (00:42):
We actually have a long history with the Leica microscopes. I've trained on them during residency, fellowship, and then also use them while out of practice. So, when it came time to upgrade our microscopes in the operating room, we naturally wanted to see what the latest technology model of the Leica microscope was. In this case, it was the Proveo 8. We got the Proveo 8 in early 2018 and we're one of the first places in the country to get it. We were impressed with its increased resolution and also its depth of focus. Also, we liked how it integrated well with the BIOM wide-angle viewing system and that process was seamless. But most importantly, we like access to new technology with the intraoperative OCT or the EnFocus system. So, we've been able to use that in a lot of our surgical practice and have been impressed with the results.
Asheesh Tewari (01:48):
So, EnFocus has been a wonderful tool for us. It's the type of tool that the more you use it, the more benefits you get with it. And in particular, we're using it for a lot of our diabetic vitrectomy cases. For some of our patients who have diabetic vitreous hemorrhage when you see them in the office, a lot of times their vision is quite limited and you're able to not get a detailed view of what their macula looks like. So, in these patients once they're in surgery and we're able to remove the blood, we can get our first glance at the macula and having the ability to do OCT on these patients gives us information regarding any presence of macular hole, epiretinal membrane, or any other tractional membranes that may be present on the surface of the retina. So, we found that to be particularly helpful for our diabetic patients.
Asheesh Tewari (02:39):
Also in cases of diabetic tractional retinal detachments, we're trying to identify planes for dissection, intraoperative OCT comes in handy. We also use it for cases of sub macular hemorrhage, where we're replacing subretinal tissue plasminogen activator. So, this helps in localization of that. Also, it can be helpful for vitreomacular traction to ensure that there's release of any traction at the end of surgery. And one of the other exciting areas is gene therapy. We're seeing more and more clinical trials with gene therapy medications that are going to be delivered in the subretinal space. So, being able to identify those spaces and ensure delivery of medication I think you'll find that intraoperative OCT will be key for that in the years to come.
Asheesh Tewari (03:34):
One of the things that I enjoy about the Proveo is the foot pedal. The foot pedal is completely customizable and I'm able to control all aspects of the microscope and the intraoperative OCT modes. I can enter in and out of. I can adjust the focus of the OCT. So, having that control all within my hands really is a very comfortable feeling. One of the other things that I enjoy about the Proveo is its visualization. The FusionOptics allow a greater resolution and depth of focus when you're doing anterior segment work, when we're working with interocular lenses. But also its integration with the BIOM wide-angle viewing system is seamless. That can allow for some improvement in workflow, simple things like the microscope light turning off when we're starting with vitrectomy, auto-inversion. These types of modes really improve our workflow.
Asheesh Tewari (04:32):
Also, the assistant scope. When you work with residents and fellows, oftentimes you may be sitting in an assistant scope, but one of the unique features with the Proveo, is that the view from the assistant scope and the view from the surgeon’s scope is identical. So, that's a really, really helpful tool. And finally, for recording, I like to do a lot of recording of surgery and video editing and having an HD camera and excellent recording system to which I can just connect an external hard drive and I can do my editing on the fly, really is efficient and high-quality.
Asheesh Tewari (05:16):
The Proveo 8 and the EnFocus OCT has helped in improving clinical outcomes and in particular for our diabetic vitrectomy cases. And as we discussed earlier, having the ability to get real-time information on the status of the macula has changed some of our surgical decision-making. In short, if it's something you're interested in, I suggest that you try it. That's one of the best things you can do is do a clinical evaluation, use the Proveo, use the EnFocus and I think you'll get a better sense of the resolution, better sense of the higher level of technology with intraoperative OCT and the more you use it, I think the more benefits you'll find with it.
Related Articles
-
RPE65 Gene Therapy Subretinal Injection: Benefits of Intraoperative OCT
Discover how RPE65 gene therapy subretinal injection procedures in patients with Leber congenital…
Feb 01, 2024Read article -
Posterior Segment Surgery: Benefits of Utilizing Intraoperative OCT
Learn about the value of intraoperative optical coherence tomography in posterior segment surgery to…
Oct 31, 2023Read article -
Improve Macular Hole Surgery with Optical Coherence Tomography
A case study on the use of intraoperative OCT during macular hole surgery for pediatric lamellar…
Aug 21, 2023Read article