Surgical neurovascular diseases overview
Prof. Bijlenga starts by talking about the dufferent types of neurovascular diseases:
- Intracranial aneurysms are the most prevalent disease, affecting around 3% of the population but the rupture of the aneurysm is a rare event with an incidence of 4 to 10 cases per 100 000 inhabitants.
- Cerebral arterio-venous malformations (AVM) are much less prevalent but more severe for affected people with a risk of rupture.
- Dural fistulas are even rarer, and the incidence of issues are very rare.
- Intracranial steno-occlusive disease (Moyamoya disease) is extremely rare.
There are many techniques to treat these diseases, including surgery, vascular treatment and radiosurgery. The treatment plan should be customized for each patient. Surgical techniques include intracranial aneurysm clipping, cerebral arterio-venous malformations resection, dural fistula clipping and Moyamoya disease revascularization.
Aneurysm clipping tools & techniques
Since the introduction of the Yasargil technique, there have been many advances in aneurysm clipping tools and techniques, improving the quality and safety of procedures. The direct puncture of the aneurysm is extremely reliable, but it can be scary for neurosurgeons to cut the dome, Prof Bijlenga explains.
Many tools that have been introduced supporting aneurysm surgery and minimizing invasiveness, each with pros and cons. These include:
- The use of endoscopes, which help to check behind the aneurysm, and in the dark angles of the operating field Endoscopes are rapid and reduce dead angles but are also bulky and subject to a limited sensitivity
- Microvascular dopplers allow to listen to the blood in the vessel and verify that there is a good perfusion in all of the branches. It also helps to check that there are no turbulence coming from stenosis. They are fast and easy to use but are subject to problems with specificity and sensitivity.
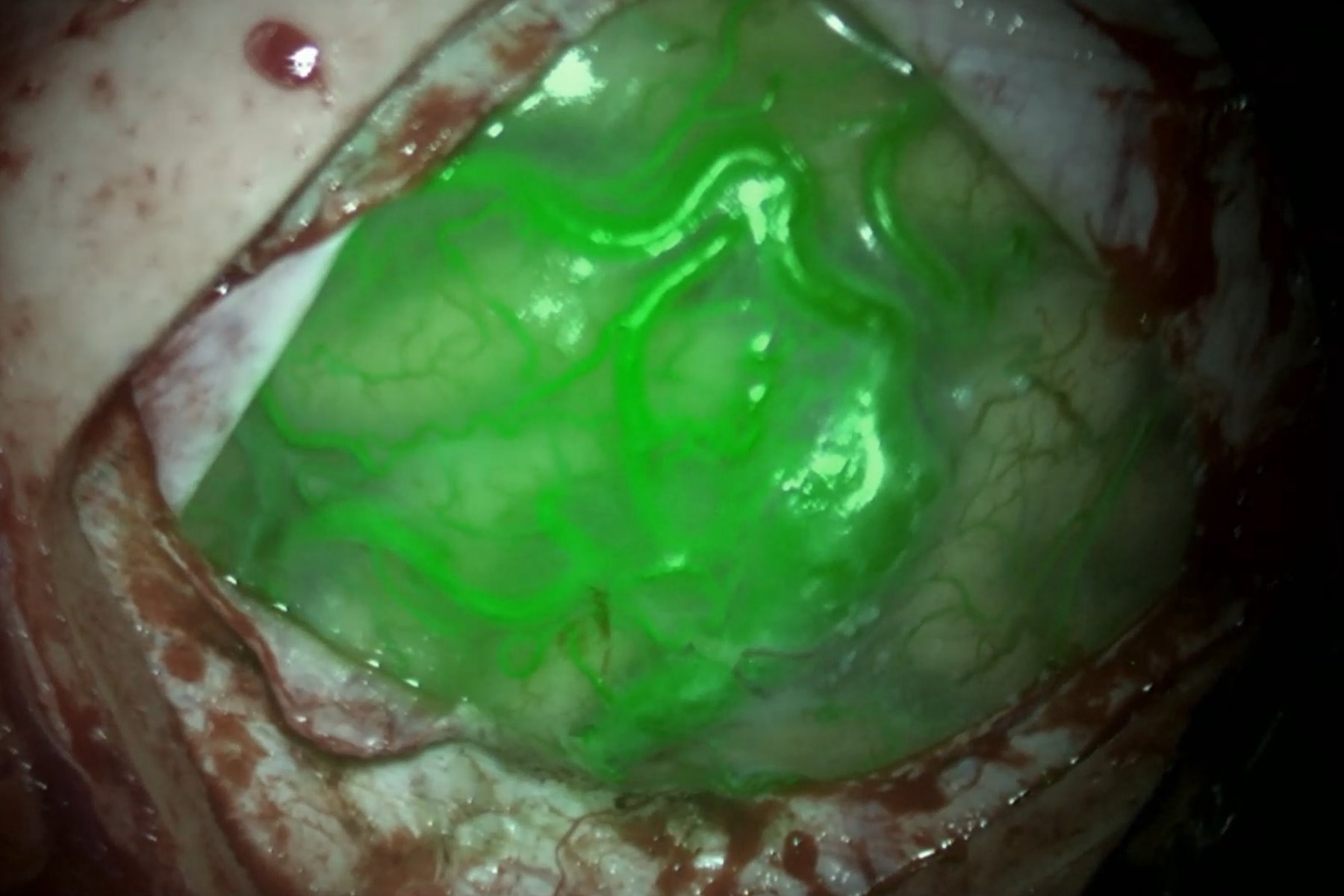
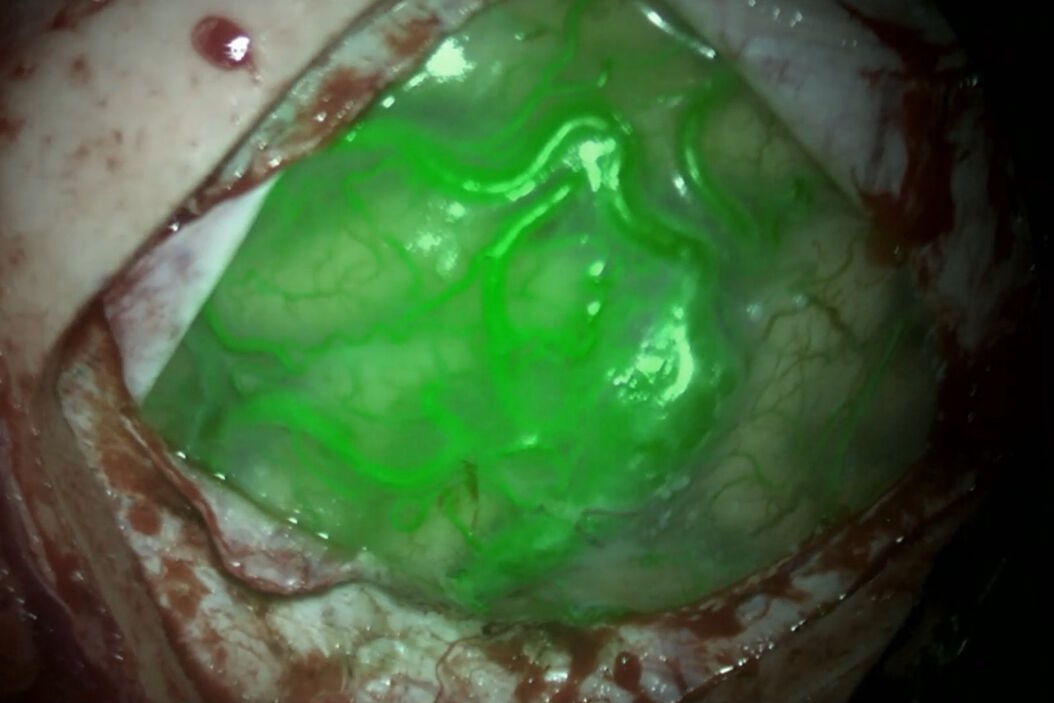
- Near-infrared indocyanine green video angiography enables the visualization of the flow of the dye in the vesssels, the flow in the vessels and that the aneurysm is excluded and that the perforators are well perfused.This tool is rapid, very easy to use and sensitive, but it requires to work in the dark with dead angles
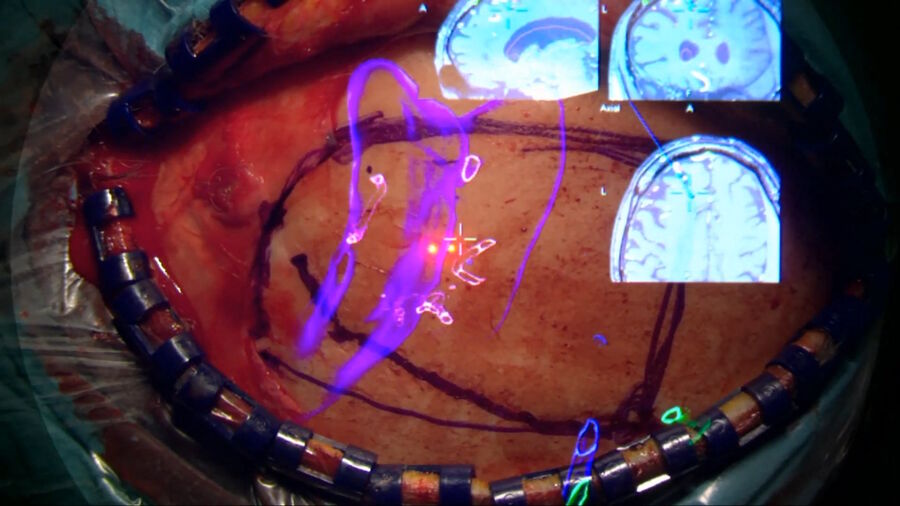
- Augmented Reality (AR) improves minimally invasive approaches, to displace the brain as little as possible and have a good representation of the anatomy to adjust the clip as precisely as possible. It facilitates the approach and clipping but it is not live information
- Endoscope-integrated indocyanine green allows to visualize the vessels with the help of Indocyanine Green and look behind the aneurysm. This reduces the dead angles of ICG angiography but it is bulky and there are still some dead angles. The issue with Indocyanine Green is that since it is near infrared, one needs to have a camera and to display the images on the screen. To do that, one needs to look away from the operating field and to remember or recognize the structures. The innovation in this istance is getting the video image back in the ocular pieces so that one can have an overlay of the fluorescent image on the visual field, similar to what GLOW800 provides today.
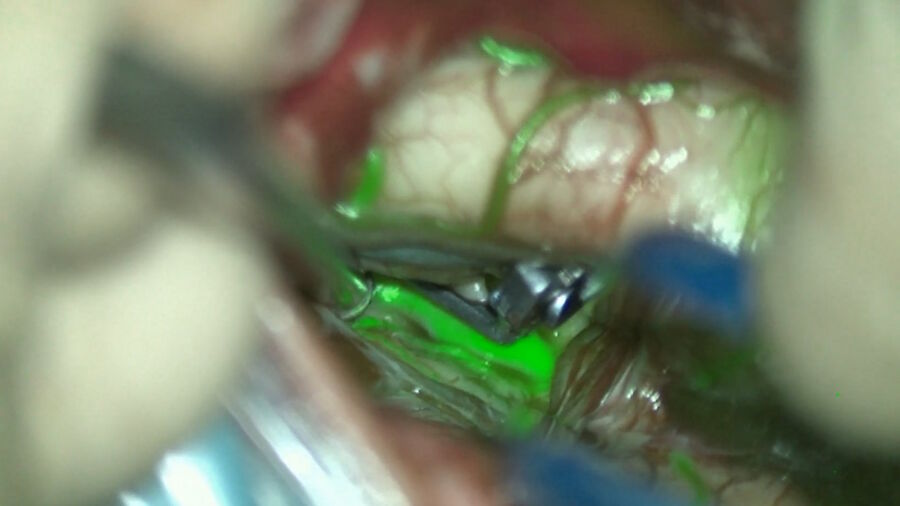
- Dual-image video angiography (DIVA), such as GLOW800 Augmented Reality, gives access to the indocyanine green fluorescence image in the operating field. It corrects the darkness of ICG angiography by having the fluorescent image of the vessels overlayed on the operating field. However, it is not as sensitive as black and white and there are a few dead angles and shadows.
- Hybrid Operating Rooms allow to perform an angiogram during the surgery, with a 3D replicate of the patient vasculature, to confirm that all vessels are preserved. It allows to control the cerebrovascular anatomy but it isn’t a very accessible and widely available technology
- Neuromonitoring is an efficient tool to monitor the function of the brain during the operation and reduce complications. It is sensitive but only has a functional impact, it doesn’t provide morphological information. Nowadays it can record the sensorimotor function of the patient, cranial nerves and enables surgeons to monitor the activity and function of the brain during the operation.
Geneva University Hospitals neurovascular surgery approach
The Geneva University Hospitals work in a Hybrid Room environment, with neuromonitoring, neuro-navigation and Augmented Reality, leveraging the Leica microscope with GLOW800 Augmented Reality navigation.
Each aneurysm clipping procedure is carefully planned with the residents based on a 3D angiogram, looking at vessels that will be used as guides and how to perform the clipping. Before the craniotomy and during the procedure, Augmented Reality helps readjust the navigation. After the clipping, GLOW800 Augmented Reality fluorescence is used to check the branches, improving the workflow and helping to improve the safety of the procedure. However, in some cases, the FL800 black and white view can be better indicated. A 3D rotational angiogram performed intra-operatively allows one to look for any remnants and ensure there are no small residues.
For AVM surgery, Prof. Bijlenga explains, the first step is to understand the AVM, studying the draining vein and ectasies, the en passant arteries, the arterial feeders and the relation of the tip and the ventricle. Augmented Reality allows us to customize the craniotomy and identify quickly the feeders from the en passant vessels. It also helps follow the AVM dissection plan by showing the contours. The use of GLOW800 Augmented Reality during the resection allows to visualize the blood flow and timing, with the FL800 mode providing confirmation that there is no remnant. A 3D angiogram is also performed is some cases.
GLOW800 Augmented Reality is a valuable tool to see which vessels are perfused and how fast vessels are perfused. In deep seated surgeries and for small vessels, the complementary use of the FL800 mode is recommended.
Do you want to learn more? Register below to watch the full webinar presented by Prof. Philippe Bijlenga and see the clinical cases he shared.
Disclaimer: “Please note that off-label uses of products may be discussed. Please check with regulatory affairs for cleared indications for use in your region. The statements of the healthcare professionals included in this symposium reflect only their opinion and personal experience and not those of Leica Microsystems. They also do not necessarily reflect the opinion of any institution with whom they are affiliated”