Moyamoya disease patient initial presentation
The patient
This case concerns a 35-year-old female patient presenting worsening neurological signs and symptoms marked by a three year history of transient episodes of visual loss in the right eye. For two of those years, the patient suffered a complete hemiparesis, and one year of right lip rhyme deviation. For ten months, she also experienced an incomplete left hemiparesis.
The patient had previously been diagnosed with Takayasu‘s arteritis and was being treated with pulse therapy and methotrexate. In addition, the patient had a medical history of systemic arterial hypertension, diabetes, dyslipidemia, and depression.
Neurological examination
The patient was fully conscious and well-oriented, with left nasolabial fold erasure and rightward rhyme deviation. She presented a left hemiparesis with brachial predominance, as well as tactile and painful hypoesthesias in the left lower limb, and allodynia in the right upper limb.
Neuropsychological assessment
The patient was right-handed. She showed alterations in size perception, as well as face perception and working memory. She displayed moderate deficits in verbal fluency and episodic-semantic verbal memory. Furthermore, the patient showed major deficits in arithmetic skills, constructive praxis, and problem-solving.
Diagnosis
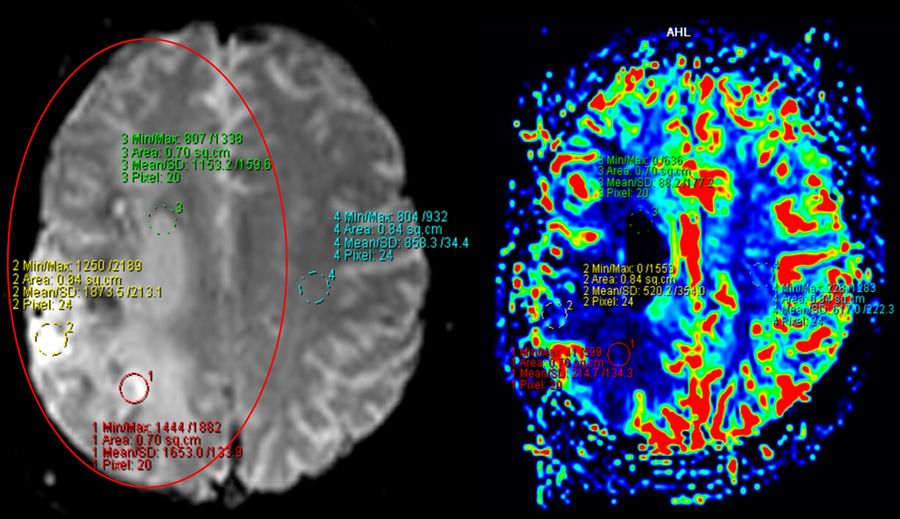
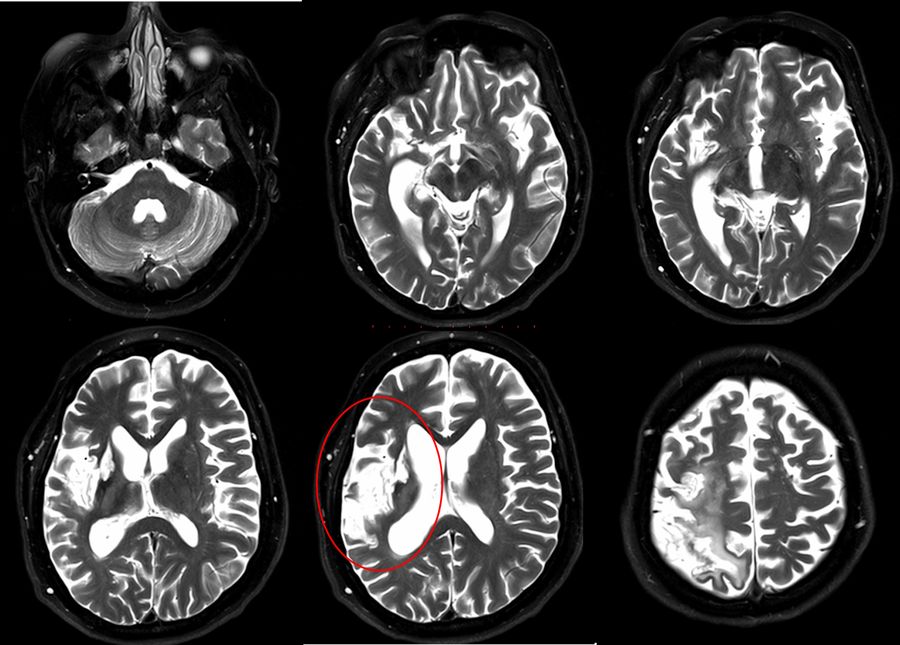
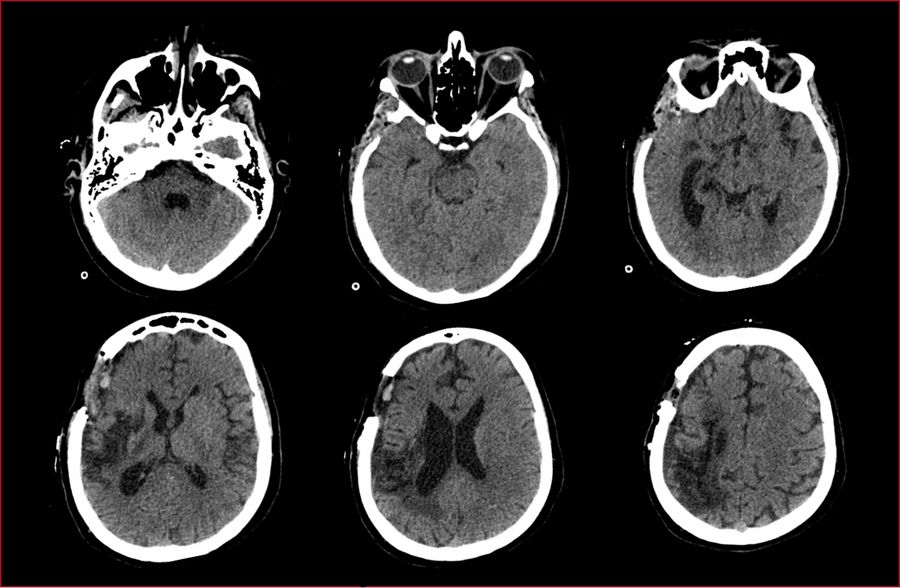
The patient was diagnosed with a stroke in the region supplied by the right middle cerebral artery caused by Moyamoya disease.
Treatment decision
The decision to perform bypass surgery was made for the following reasons:
- Worsening stroke symptoms in the right middle cerebral artery territory
- Identification of suitable bypass location that would provide adequate perfusion
Pre-operative assessment
Moyamoya disease is a chronic occlusive cerebrovascular disease characterized by progressive stenosis in the terminal portion of the internal carotid artery and an abnormal vascular network at the base of the brain.
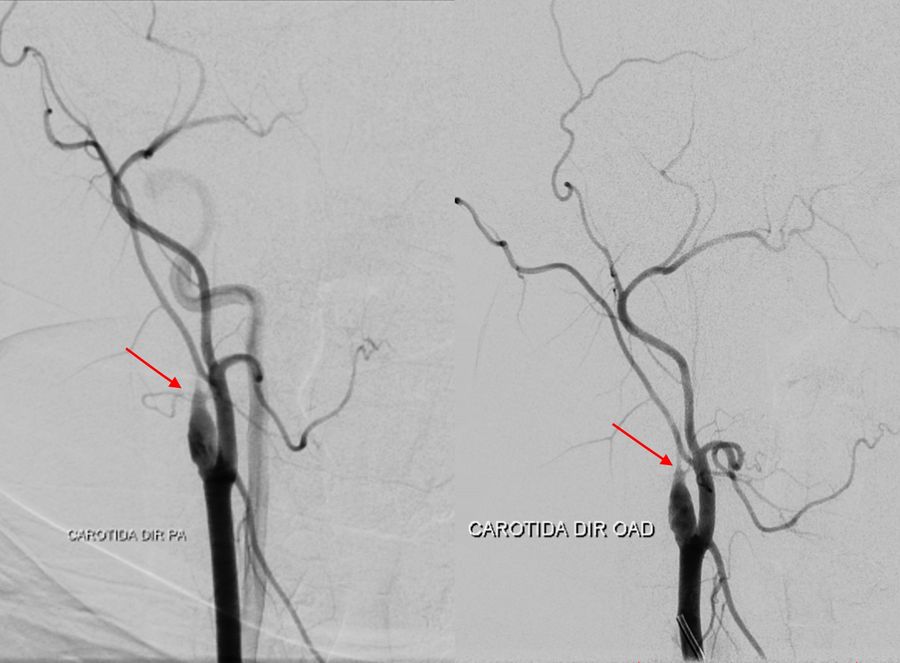
Catheter angiography was performed with the following findings:
- Occlusion at the proximal third of the cervical segment of the right internal carotid artery
- Stenosis of the supraclinoid segment of the left internal carotid artery
- Proximal stenosis of the anterior and middle cerebral arteries with collateral «smoke puff» vessels, which are characteristic findings of moyamoya disease
- Collateral circulation from the internal maxillary artery to the ipsilateral carotid territory
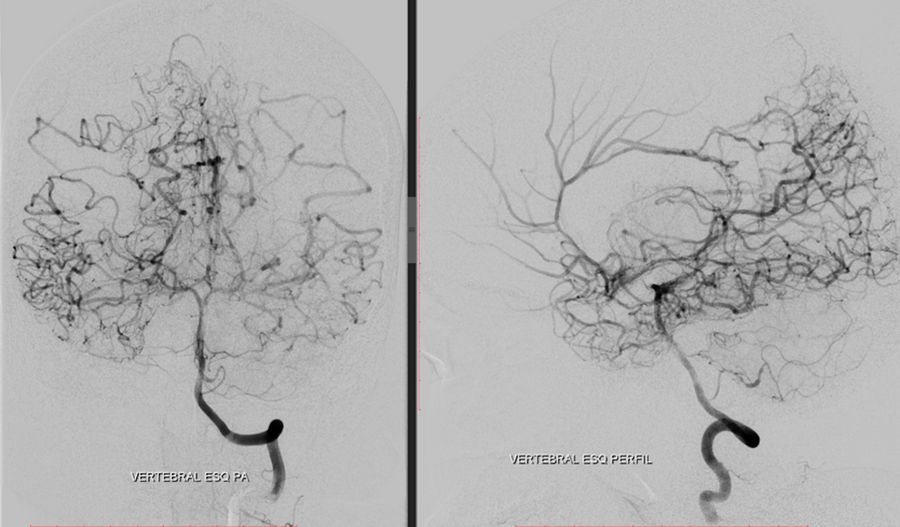
- Collateral irrigation of the carotid territory from the posterior circulation through a patent posterior communicating artery
A DSA (digital subtraction angiography) was performed pre-operatively to assess the occlusions of the internal and external
carotid arteries, as well as stenosis of the arteries and the feeding and draining blood vessels of the arteriovenous malformation, as
shown in the images below.
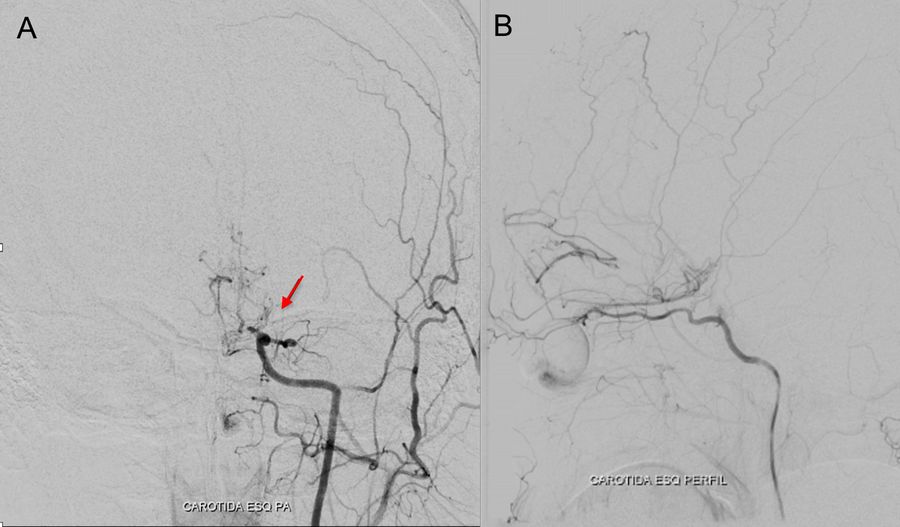
middle cerebral arteries and collateral vessels as a “puff of smoke” which are characteristic findings in the context of moyamoya disease (Scott, R. M., & Smith, E. R. (2009)). B: Image of the left external carotid artery showing the collateral circulation from the internal maxillary artery to the ipsilateral carotid territory.
Intra-operative course and images
The patient was placed in the supine position, with the head fixed with three-pin support. Preparation for the procedure and dissection of the temporal artery was initiated. A semi-curved incision centered on the left temporal region was made. The musculocutaneous dissection of the temporal muscle was performed using self-retaining retractors to expose the pterion. Subsequently, a pterional craniotomy was performed and after opening the dura, the inferior frontal gyrus, the superior temporal gyrus, and the Sylvian fissure were exposed. Finally, the subarachnoid dissection through the Sylvian Fissure was continued, to select an adequate branch of M4 to be the receiving artery.
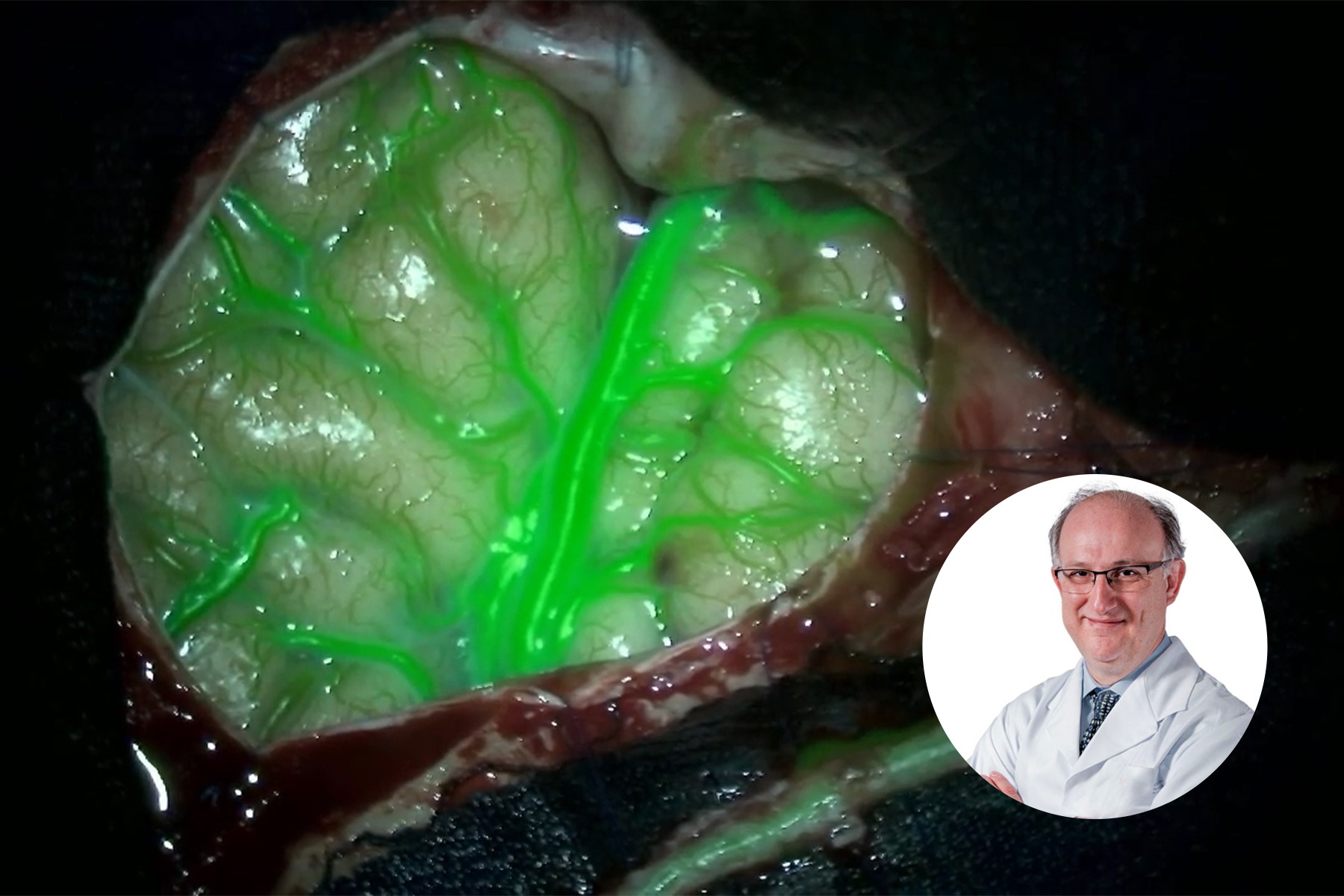
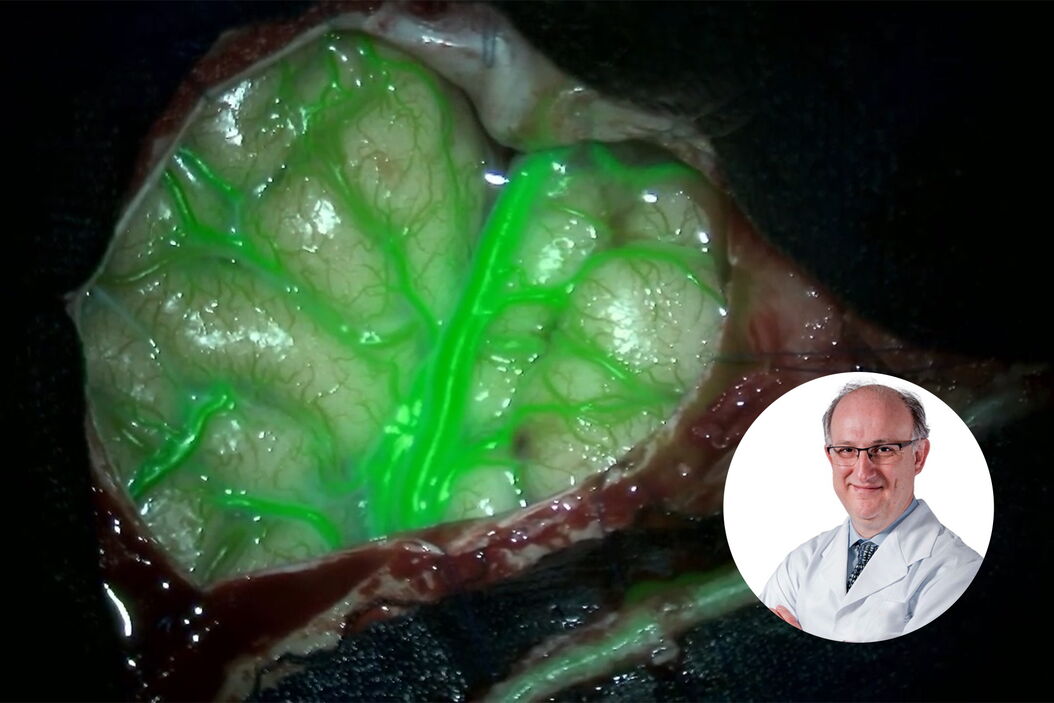
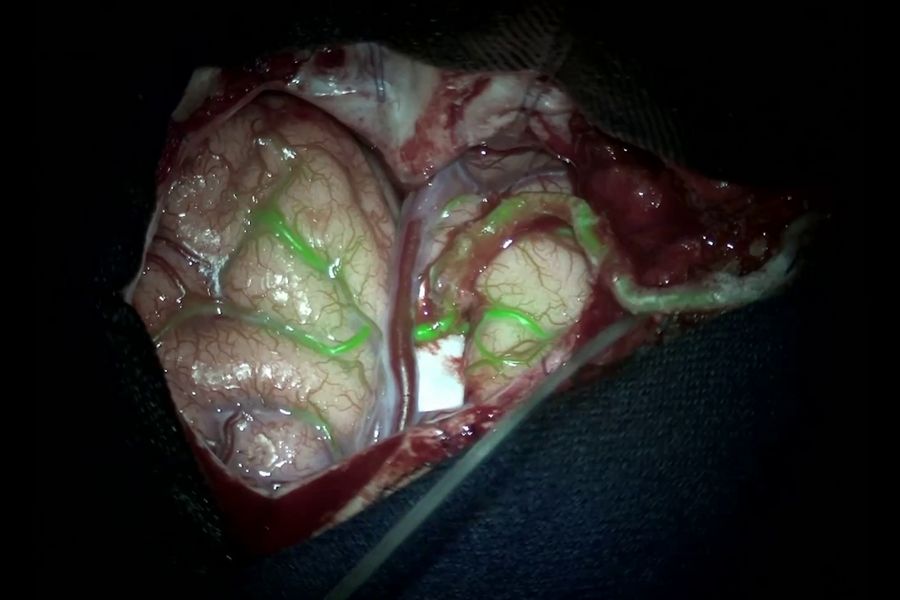
During the first step, a superficial artery dissection was performed (Video 1) and the blood flow through the artery was assessed using GLOW800. Following the dissection of the superficial temporal artery, an additional check with GLOW800 for potential hemorrhaging and thrombosis was performed.
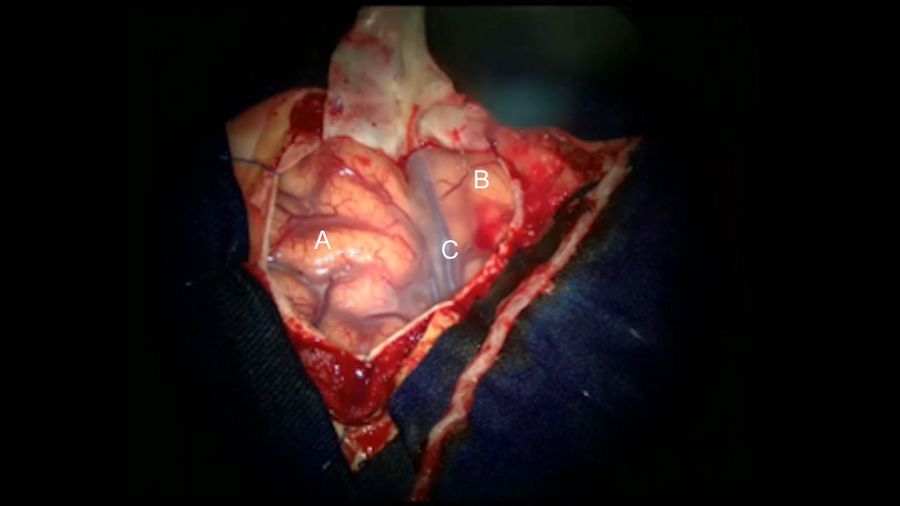
Subsequently, a pterional craniotomy (shown in Figure 8) was performed to expose the frontal inferior gyrus (A), the superior temporal gyrus (B), and the Sylvian fissure (C). Fig. 9 and Video 3 depict the subarachnoid dissection through the Sylvian fissure, where the M4 branch crossing the temporal gyrus was chosen to be assessed as the receiving artery due to its proximity to the Sylvian fissure and the suitability of its diameter.
Prior to the anastomosis, GLOW800 was used to assess the cerebral blood flow through the feeding arteries and the M4 branch, helping to determine whether it is patent and has an adequate diameter. After the assessment was completed with a good outcome, the anastomotic mouth of the temporal artery was performed for the bypass, as demonstrated by Fig. 11 and Video 5.
In the next stage of the surgery, after the clipping of the proximal and distal segments of the M4 branch of the MCA, the receptor M4 branch was prepared for the bypass, as demonstrated in Fig. 12 (Video 6). In Fig. 13 (Video 7), the anastomosis between the superficial temporal artery and the receptor M4 branch was performed.
After the bypass was performed, GLOW800 was essential to the assessment of patency of the arteries, as well as for ensuring the absence of hemorrhages and thrombosis, allowing for the identification and correction of the immediate causes of failures in the anastomosis.
Post-surgery assessment
The postoperative CT scan showed no signs of postoperative complications. The presurgical area of ischemia in the territory the right MCA was also observed. The patient showed no additional postoperative neurological deficits and was discharged three days post-surgery.
Impact of glow800 augmented reality fluorescence in moyamoya disease treatment
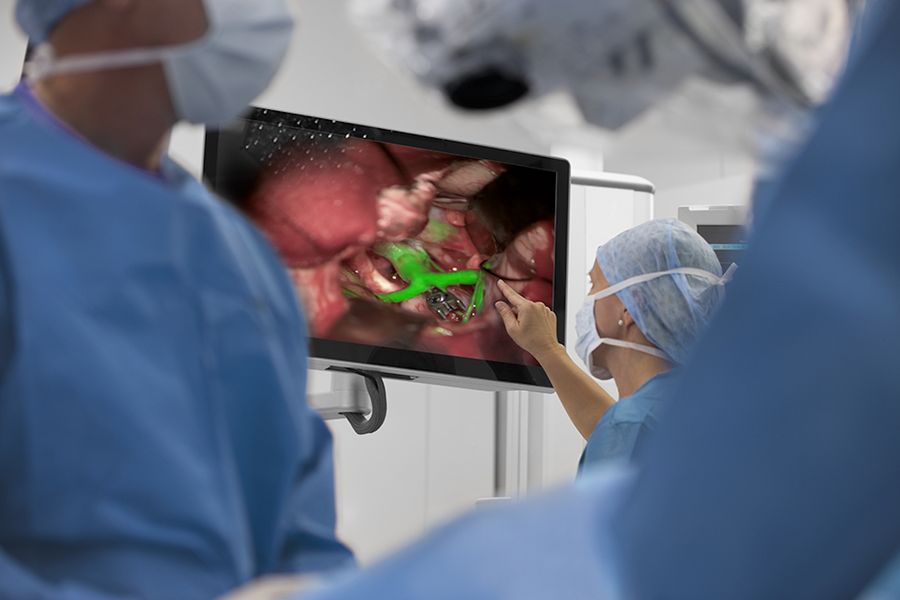
One augmented view during vascular neurosurgery improves confidence in intraoperative diagnosis
- Having a single augmented, real-time view means there is no need to recall and try to reconcile the black and white blood flow video with the natural anatomical view.
- Crisp delineation helps you limit potential compromise and obstruction of surrounding perforators and small vessels. > Full depth perception and the absence of dark peripheries ensures clear spatial orientation to aid precise manipulation of vessels.
Improved confidence in treatment
Visualization with GLOW800 AR supports each step of vascular neuro-surgery procedures, as well as postoperative imaging. Specifically, during bypass surgery, GLOW800 provides the following advantages:
- Accurate assessment of blood flow through the feeding and receiving vessels, aiding in their selection.
- Identification of the presence of thrombosis or stenosis of vessels before anastomosis.
- Intraoperative assessment of the patency of anastomosis, as well as of the presence of thrombosis or stenosis.
- Intraoperative assessment of blood hemorrhage through anastomosed blood vessels, including kinking and partial obstruction.
The use of GLOW800 Augmented Reality fluorescence provides one augmented real-time view during vascular neurosurgery. Neurosurgeons do not need to recall and try to reconcile the black and white blood flow video with the natural anatomical view. The crisp delineation, full depth perception and absence of dark peripheries supports precise manipulation of vessels.
Benefits of GLOW800 Augmented Reality
With GLOW800 Augmented Reality, it is possible to:
- Perform an accurate assessment of blood flow during bypass surgery through the feeding and receiving vessels, aiding in their selection
- Identify the presence of thrombosis or stenosis of vessels before anastomosis and do an intraoperative assessment of the patency of anastomosis
- Intraoperatively assess blood hemorrhage through anastomosed blood vessels, including kinking and partial obstruction.
As such, GLOW800 supports Moyamoya disease treatment and outcomes and is a fundamental tool for the future of practice and training in neurosurgery. Want to learn more? Register below to download the full case study and access the clinical videos.
Acknowledgements
All clinical images and videos supplied for this report are courtesy of Prof. Dr. Feres Chaddad, Head of Vascular Neurosurgery at the Federal University of São Paulo (UNIFESP), São Paulo, Brazil.
Leica Microsystems would like to thank the University of São Paulo for its collaboration on this case study, and especially Prof. Dr. Feres Chaddad for his work on this report.
Note: The statements of the healthcare professional in this case study reflect only his opinion and personal experience. His statements do not necessarily reflect the opinion of any institution with whom he is affiliated. Please check with your local Leica Microsystems representative for product registration status in your region.