Dr. Romain Bosc, a Plastic, Reconstructive and Cosmetic Surgeon at the Henri Mondor Hospital in Créteil, France, looks at how each of these technologies support surgeons and the role they can play. He explores the benefits and cases in which they are particularly useful, to reduce complications and improve outcomes.
Dr. Bosc also discusses the future of reconstructive surgery, and the emerging groundbreaking technologies currently being tested. These innovative solutions, such as smart glasses with Augmented Reality, Artificial Intelligence for computer-assisted decision-making, robot assistance and telesurgery remote guidance, could further augment surgeons’ abilities.
Introduction
Technological advances have the power to revolutionize surgical practice, as shown by the history of medicine. Very early on, surgeons faced the limitations of their sensory capacities. With the introduction of binocular loupes and microscopes in the operating room, their visual capacity has been
significantly enhanced.
Later on, analogue imaging, followed by digital imaging, gave surgeons the ability to view, on screens, the results of radiological investigations carried out on the patient. This digitization of radiological imaging, combined with the exponential increase in computer processing capacities, has paved the way for three-dimensional reconstructions, computerized planning, computer-aided design, 3D printing and augmented reality (AR).
Nowadays, all these techniques and technologies are part of decision-making and patient care in reconstructive surgery.
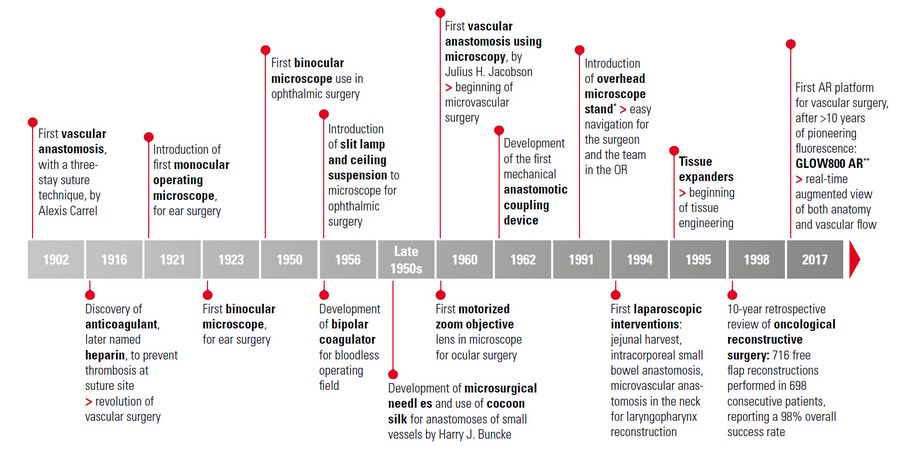
Microsurgery evolution: Key technological milestones throughout the years
Over the last century, important technological advances have contributed to the development of microsurgery. Thanks to these advances, surgeons have been able to enrich their skills and surgical techniques, and to operate on increasingly smaller anatomical structures with greater precision and
success [1].
Oncological reconstructive surgery: Surgical assistance technologies improving outcomes
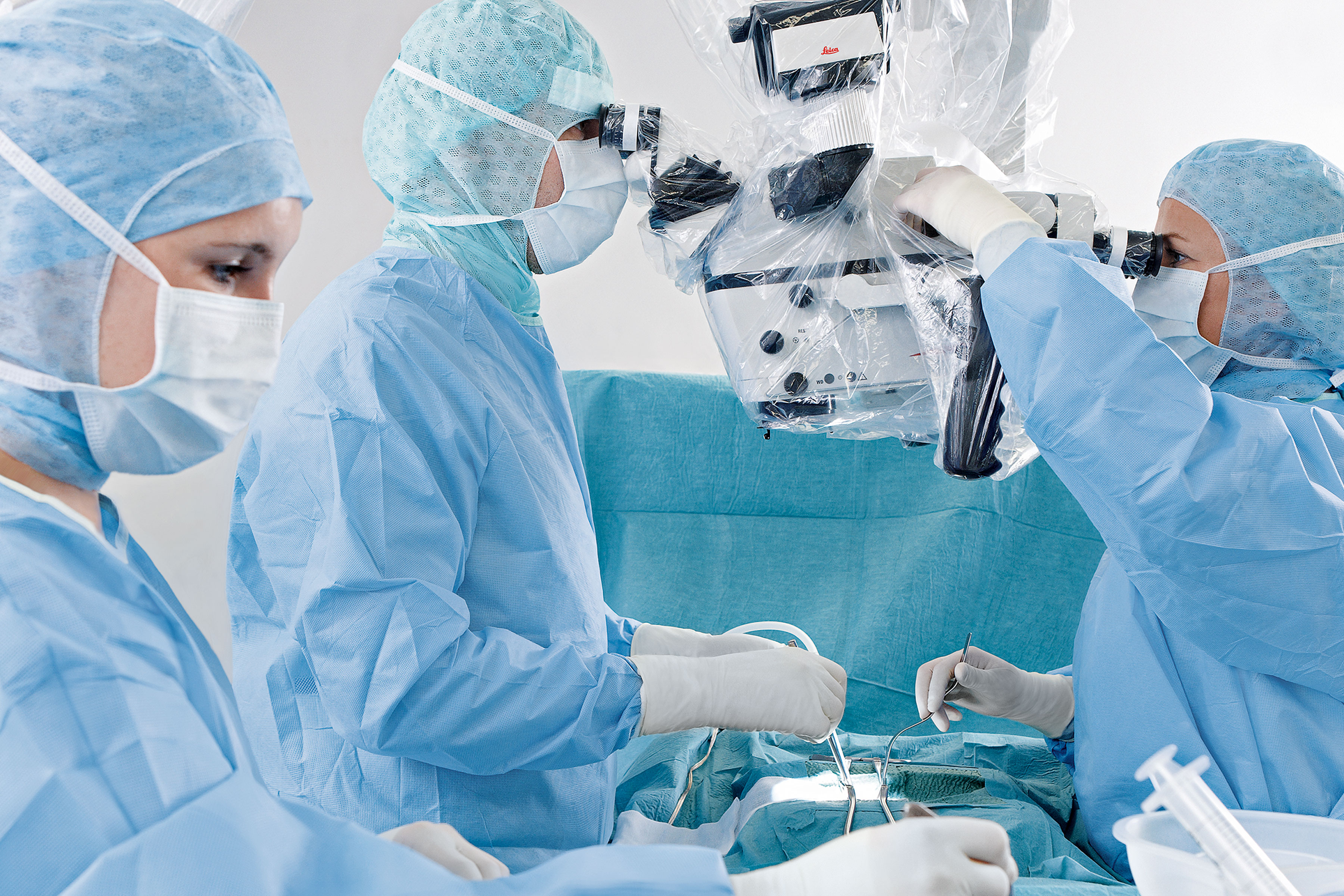
Today, surgeons have access to several technological innovations helping them in the OR. These innovations improve ergonomics and visualization capabilities during surgical procedures and allow to better plan the surgery. In addition, it is easier to share the surgical view with students and peers.
Ergonomic visualization posture avoiding musculoskeletal problems
The use of adjustable microscopes offers an adequate level of magnification of the operating field while allowing the surgeon to maintain a neutral neck posture [2]. With some microsurgical microscopes surgeons can even define their own ideal operating position, through the eyepieces or heads-up looking at the screen.
In addition, with ergonomic microscopes, it is possible to accurately adjust the working distance, zoom and field of view as needed, for both close visualization of anastomosis and wide view of flap perfusion, in high resolution, and without letting go of surgical instruments.
The assisting team benefits from a clear, sharp view while avoiding inappropriate positioning and reducing the risks of infection and sepsis.
The use of the microscope binoculars for the surgeon’s assistants allows visualization with the same image quality, ensuring alignment on the progress of the surgery.
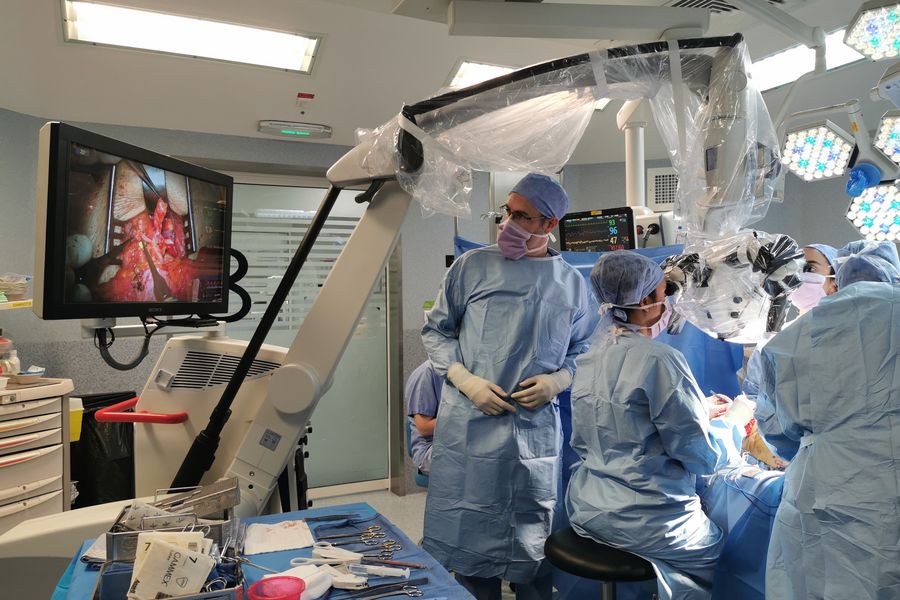
The introduction of 3D stereoscopic video displays has reduced forward head posturing during microsurgery while enhancing team engagement in the operation, as these displays make the operating field visible to all in the OR [3]. Leaders in the development of ergonomic optimization, such
as Leica, have developed microscopes that allow the team to visualize every step of the surgery on HD/4K screens, in 2D or 3D, with long arm reach and a small footprint inside the OR, thereby ensuring optimal surgical workflow.
- Plastic surgeons are at HIGHER RISK OF WORKRELATED MUSCULOSKELETAL ISSUES.
- The most frequently affected regions are the NECK, SHOULDERS AND LUMBAR SPINE.
- Up to 87% of surgeons report NECK AND SHOULDERS MUSCULOSKELETAL SYMPTOMS.
- The use of loupe magnification INCREASES THE MEAN CERVICAL LOAD BY 40%
Indocyanine green (ICG) fluorescence assessing anastomosis and flap viability
For patients with cancer, post-cancer reconstruction of breast or head and neck is essential. The development of imaging technologies has contributed to making these procedures safer and more reliable.
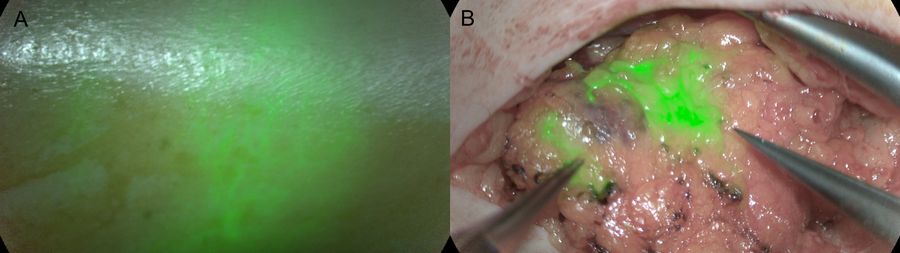
The use of cameras to detect indocyanine green (ICG) fluorescent intravenous dye enables the assessment of poorly perfused areas of the free flap or the mastectomy skin flap as well as the evaluation of microvascular anastomosis. As a result, postoperative complications are reduced, including the rate of flap necrosis and the risk of flap loss [3,4].
As an example, Leica’s near infrared visualization technology integrated within the microscope can easily detect ICG infused blood flow and tissue perfusion in real time, without interruption of the surgery or need for additional devices in the operating area. Users benefit from both high magnification and visualization comfort provided by the microscope.
Cutting guides and 3D printing improving difficult reconstructions
Head and neck reconstructive surgery largely relies on the use of free flap techniques such as vascularized fibular flap. Transforming the fibular bone into a 3D structure with angulations specific to each patient is often challenging. Computer-assisted preoperative planning can help overcome this difficulty. Computer-designed customized cut guides can be made by the surgeons themselves using 3D printing technology with approved biocompatible materials leveraging open-source freeware or provided by manufacturers. This approach contributes to a better understanding of each surgical case, decreasing the risk of modelling errors and the duration of the intervention while increasing the quality of the reconstruction [5,6].
AR and high magnification facilitating microsurgery interventions and challenging cases in particular such as lymphoedema surgery
Lymphoedema affects approximately one in seven cancer patients [7]. Different surgical interventions efficiently reduce lymphoedema, but their practice has been restricted by surgeon/equipmentrelated factors and their effectiveness has been limited by technical constraints [8]. Recent technical advances in microvascular surgery facilitate these procedures:
- The detection of ICG using a microsurgical microscope equipped with a high magnification option enables microsurgery on small lymphatic vessels (0.3-0.7 mm) [9]. The FL800 fluorescence visualization technology and the Magnification Multiplier options, integrated into the microscopes,
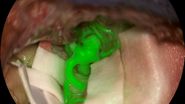
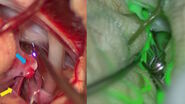
help meet the needs of microsurgery. - The use of vascular AR fluorescence offers both visualization of anatomy and fluorescent view of vascular flow, in real-time and in OR ambient light. The AR feature enables lymph node detection, removal, anastomosis and validation of effectiveness without interruptions in the surgical
workflow or the need to switch off the light in the OR [9]. The breakthrough GLOW800 patented AR technology is not only useful for lymphoedema surgery, it is a game-changing solution providing superior insights for every type of vascular reconstructive surgery procedure.
2D and 3D video recording for training and teaching purposes
Recent 2D and 3D cameras development or progress on microsurgical microscopes have contributed to a shift in medical education and how anatomy is taught. Visualization of real intervention videos and tutorials in 3D enhance students’ fundamental anatomical knowledge, anatomical relationships and reasoning. Some universities offer this type of training and students enjoy being able to view the surgery from the operator’s perspective [10]. It also means that surgeons can share the HD images and surgical videos captured by 2D or 3D cameras with their students, their assisting team in the OR or with their peers at meetings, by displaying them on HD/4K screens.
The future of reconstructive surgery: Innovations paving the way
Groundbreaking technological innovations are currently being tested, with the potential to enhance the surgeon’s abilities even further.
Smart glasses with AR within see-through projection systems
The latest AR innovations greatly facilitate surgical interventions however, ideally, AR technology should be incorporated into surgical glasses or headsets. This would allow the surgeon to have a 3D view of the surgical field with other digital information right infront of his eyes to perform surgery with both hands free. The addition of a tracking system as well as the improvement of sensor quality and miniaturization could provide an ‘augmented’ visualization of the operating field surpassing the surgeon’s naked eye. This 100% hands-free AR enhanced and magnified visualization of the surgical field could be adopted by surgeons for different types of reconstructive procedures, including free flap reconstructions and removal of non-palpable tumors [11].
Robot assistance overcoming human limitations
Lymphatic supermicrosurgery remains one of the most challenging procedures due to the small diameter of lymphatic vessels. Different teams of surgeons, scientists and engineers have tried to design robotic systems able to perform reconstructive microsurgery. So far, surgical robots have not yet succeeded in improving the surgeon’s abilities for complex microsurgical procedures. However, other robotic systems that help stabilize movements of the microsurgeon filtering tremors and scaling down motions are currently being tested in lymphovenous anastomosis supermicrosurgery procedures. As of today, roboticassisted lymphovenous anastomosis has proven feasible, with similar benefits to manual surgery in terms of patient outcomes, raising the hope for promising results in the future. However, large multicenter trials are needed to confirm these benefits and further demonstrate the therapeutic value of robot-assisted supermicrosurgery [12]. Moreover, the transition to robotic systems will take time and surgical microscopes can help facilitate the shift allowing surgeons to build confidence and embrace the possibilities of technology in the OR.
Artificial intelligence for computer-assisted decision-making
Digital advances in artificial intelligence (AI) algorithms are being incorporated in different technological fields. In microsurgery, AI could contribute to the analysis and concomitant integration of different data sources indicating the patient’s vital status before and during the surgery. This could help anticipate medical issues before they occur and potentially predict complications during or after the surgical procedure [13].
Telesurgery remote guidance
The culminating example of future possibilities in microsurgery is the use of telemedicine in the OR: surgeons located in distant places could remotely guide their peers throughout the procedure, or even operate on the patient themselves by using robotic assistance [13].
Conclusion
The digitalization of both radiological imaging and the surgeon’s visual environment, associated with microscopy, have considerably improved the practice of reconstructive microsurgery and the safety of procedures. Hybrid ORs enable tomographic imaging with 3D real-time visualization of
the patient’s anatomy. The next revolution will most probably be the combination of these technologies with AR.
In the near future, the enhanced power, ergonomics and quality of AR visualization technologies should give the surgeon the ability to operate heads-up and hands-free, with digital information directly integrated in the visual field.