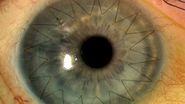
Analyze the microscope’s environment
Before selecting an ophthalmic microscope for cataract procedures and other anterior segment surgeries, it is useful to look at the set-up of the practice or clinic as well as the requirements of the surgeons who work with it.
- Where will the microscope be used? Will it be used in a small or medium-sized practice or in a large clinic? How many procedures will be performed with it on a daily, weekly, or monthly basis? How many surgeons will perform surgeries with the microscope?
- Which purpose does the microscope serve? Which range of procedures shall the microscope cover? Is it dedicated to cataract surgery only or will it also be used for other anterior or posterior procedures? Will it be the only ophthalmic microscope in the clinic or is it maybe one of several? Are there any specific requirements, e.g., does the clinic have a focus in teaching?
- Are there any plans to change the focus of the clinic, e.g., by expanding the services offered, considering the integration of intraoperative OCT, documentation, or teaching capabilities?
- Last, but not least: What budget will be available for the acquisition?
Look at what really matters in cataract surgery
Optics
The quality of the optics is key for image accuracy and thus a prerequisite for successful outcomes. High-transmission optics enable surgeons to work at lower light levels and enhance patient and surgeon comfort alike. Great depth of field contributes to efficiency in the OR. Surgeons need to refocus less, can concentrate on the procedure uninterruptedly and save time during surgeries.
Illumination
Procedures at low light level are less stressful for the patient as well as for the surgeon’s eyes. Direct illumination reduces the illumination wattage and enhances low-light capabilities. A bright and stable red reflex is key to optimal visualization of lens structures and therefore a prerequisite for positive outcomes
Factors to consider explained in more detail
Patient comfort
Patients will in all probability rarely look forward to a surgery as such, even if they desire the improvement in vision that the procedure is designed to bring about. Positive surgical outcomes are an important factor in patients’ judgements of surgeries. Yet, providing patients with a good experience before, during, and after their cataract surgery can support your practice’s or clinic’s reputation. Enhancing patient comfort as much as possible may pay off in recommendations of your practice or clinic. The choice of a suitable ophthalmic microscope does play a role: Illumination and optics contribute to patient comfort by enabling surgeons to work at low levels of light and in a smooth workflow, thus reducing stress for the patient.
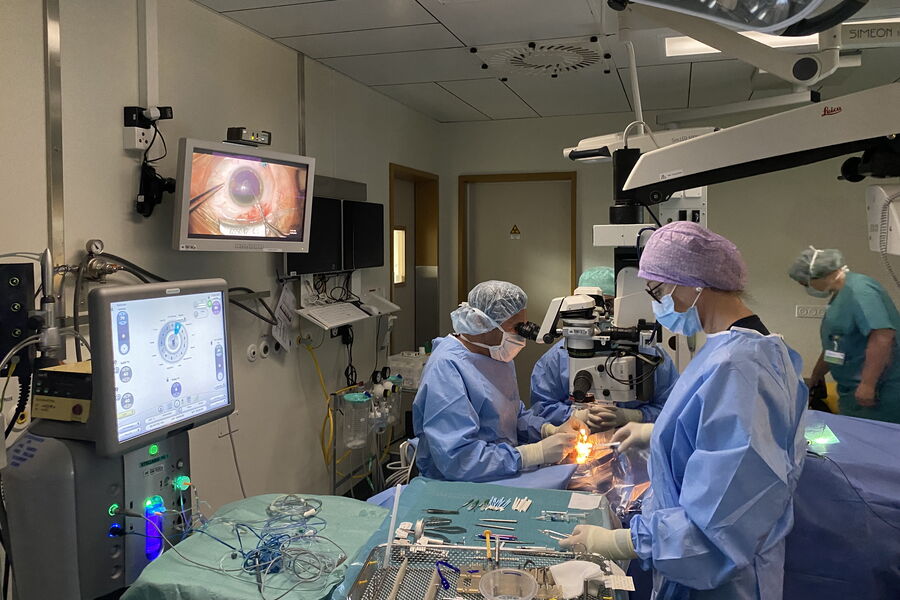
Optimal Illumination for surgeon and patient
If surgeons can work at a low level of illumination, the surgery is less stressful on their eyes as well as on their patient’s. This is a major factor for patient comfort. Surgeries are conducted with the patient’s pupil dilated under topical anesthesia, so that the patient will not feel any pain, but will still be blinded by the light, as the retina is exposed to the microscope’s illumination. Since reducing light intensity enhances surgeon and patient comfort alike, as well as the risk of phototoxicity effects on the patient retina, it is a good idea to look at the technology of the illumination.
Many microscopes use fiber optics for their illumination, which means that the light travels from the light source in the microscope body through the fibers to the optics carrier. Leica ophthalmic microscopes use direct illumination: the light source is integrated in the optics carrier. This shortens the distance the light must travel and reduces the wattage needed considerably: Conventional microscopes need light sources with around 180 Watt, while Leica microscopes such as the Proveo 8 work with less than 25 Watt. Thanks to direct illumination, Leica microscopes can be operated at particularly low light levels of around 10 to 15% of their luminous power, depending on the patient’s eye condition.
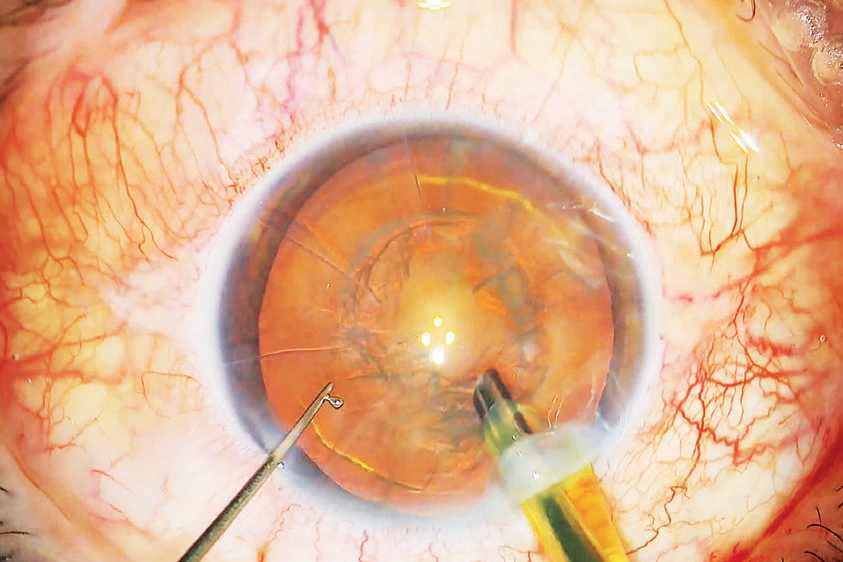
A bright and stable red reflex is crucial to distinguishing structures in the patient lens. The ability to discern these structures enables surgeons to work precisely while incising the cornea, breaking, and extracting the cataract as well as positioning the intraocular lens. The red reflex is created by light reflected by the retina. Reflections are optimal if light hits the retina perpendicularly. To enable this, the M822 ophthalmic microscope, by way of example, has two coaxial beam paths, while the Proveo 8 ophthalmic microscope has four.
The red reflex facilitated by the Proveo 8 so-called CoAx4 Illumination is the brightest and most stable in the Leica family of ophthalmic microscopes, while all Leica ophthalmic microscopes provide a bright red reflex even at low light conditions. Since there are various illumination technologies, it is therefore always advisable to compare microscopes in terms of red reflex quality.
If surgeons are interested in the flexibility to enhance and reduce contrast as needed, it makes sense to look for an adjustable red reflex illumination diameter. A larger diameter makes up for eye movement while a smaller diameter minimizes sclera reflections and enhances the contrast during surgery. The Proveo 8, for instance, offers an adjustable diameter of 4 to 23 mm.
High-quality optics for optimal visualization and a smooth workflow
The quality of the optics determines the clarity of the image a surgeon sees during procedures. Since seeing an accurate image of the patient eye is crucial to the possible success of a surgery, surgeons should look for apochromatic optics in their future surgical microscopes. Apochromatic optics are corrected for optical aberrations which occur when light passes a lens.
The quality of the optics also influences the low-light capabilities of an ophthalmic microscope. Part of any light which enters the optics is reflected by the lenses. The design of the optics as well as the material and the coating of the lenses determine how much light passes through. High-transmission optics will perform better under low-light conditions than conventional optics, simply because more of the light that enters the microscope optics also exits them to illuminate the operating site.
Leica Microsystems manufactures their optics from scratch – from the lenses to the coating. The optics for the ophthalmic microscopes are designed to reduce loss in light intensity due to scattering, thus enhancing the light transmission. This means that surgeons can in fact work at low light levels with Leica ophthalmic microscopes, always bearing patient comfort in mind.
The depth of field a surgical microscope provides, influences the workflow of the procedure. The greater the depth of field, the less often surgeons need to refocus, thus being able to work without interruptions. Smooth procedures in turn increase efficiency and enhance patient comfort alike.
FusionOptics is a technology unique to Leica microscopes. It enhances depth-of-field perception by using the ability of the human brain to merge two images into one: FusionOptics use one beam path to provide an image with a great depth of field and one with high resolution. The human brain creates a highly resolved image with great depth of field, which reduces the need to refocus during procedures. FusionOptics is currently built into Proveo 8 ophthalmic microscopes.

Ergonomic design for less physical strain on the surgeon
Very often, surgeons perform one cataract surgery after the other, sometimes even using several operating theaters for efficiency. The working posture in the OR can put strain especially on the neck and shoulders and result in musculoskeletal pain. Ergonomic accessories help to reduce this strain and enable surgeons to work more comfortably.
Leica surgical microscopes can be used with a variety of ergonomic binoculars which influence the viewing position during procedures. When choosing a new ophthalmic microscope, surgeons should try it out and pay special attention to the posture they work in – they will feel the benefit later.
Nowadays, ophthalmic microscopes can be operated in a variety of ways to adjust to surgeon and OR team preferences. A wireless footswitch is a useful accessory. It can be programmed to save settings from several users and be operated by tapping it with a foot. This avoids unnecessary movement in the OR and reduces workflow interruptions which might be caused by setting changes.
Some microscopes offer the option to program settings such as magnification, focus, and illumination for frequently reoccurring surgical phases. Leica Microsystems offers this option in the M822 with the Step Cycle function and in the Proveo 8 with Combination Mode. This supports a smooth workflow in the OR, can reduce procedure duration and can thus enhance patient comfort. This option also enhances efficiency for the entire OR team, as the settings can be selected with the surgeon’s profile before each procedure.
Low cost of ownership, smooth maintenance workflow
Considering the budget for a new surgical microscope should also take maintenance into account. Depending on how much an ophthalmic microscope with fiber optics is used, the optical fibers may need to be exchanged. They wear with every movement of the microscope arm, as they span the distance from the microscope body to the optics carrier. This movement may result in tiny damages to the fibers, thus affecting illumination intensity over time. As a result, surgeons may need to increase the illumination values to be able to maintain the brightness and visualization quality. If the visualization quality is no longer sufficient, optical fibers may need to be exchanged.
Direct illumination reduces cost of ownership as the illumination source is in the optics carrier with no fibers needed. With a lifetime of approx. up to 50,000 hours in LED, there is no need to exchange the lamps of Leica ophthalmic microscopes during their lifetime.
If a surgical microscope is easy to clean, it takes less time to do so for the OR staff. Watch out for nooks and crannies – flat surfaces and internally routed cables are better suited to easy cleaning. Antimicrobial coating of surfaces also helps enhance hygiene. Last, but not least, anything that can be removed to be sterilized, such as handles or covers, should be made from durable materials to ensure longevity.
Upgrade options
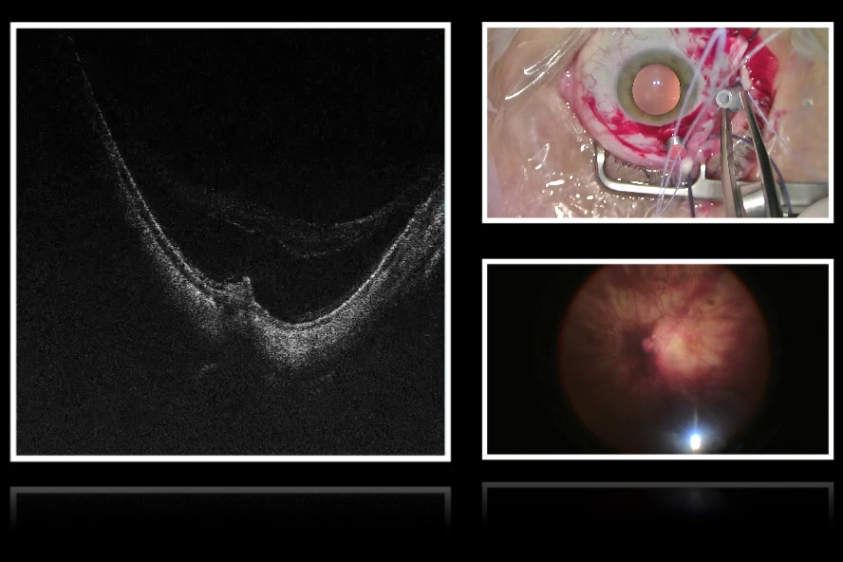
Depending on the present and future set-up of the clinic, it may be worthwhile to consider the upgradeability of the ophthalmic microscope. E.g., if the use of the microscope shall be extended beyond cataract surgery to cover further anterior or posterior procedures, options to integrate intraoperative optical coherence tomography (OCT) may become important.
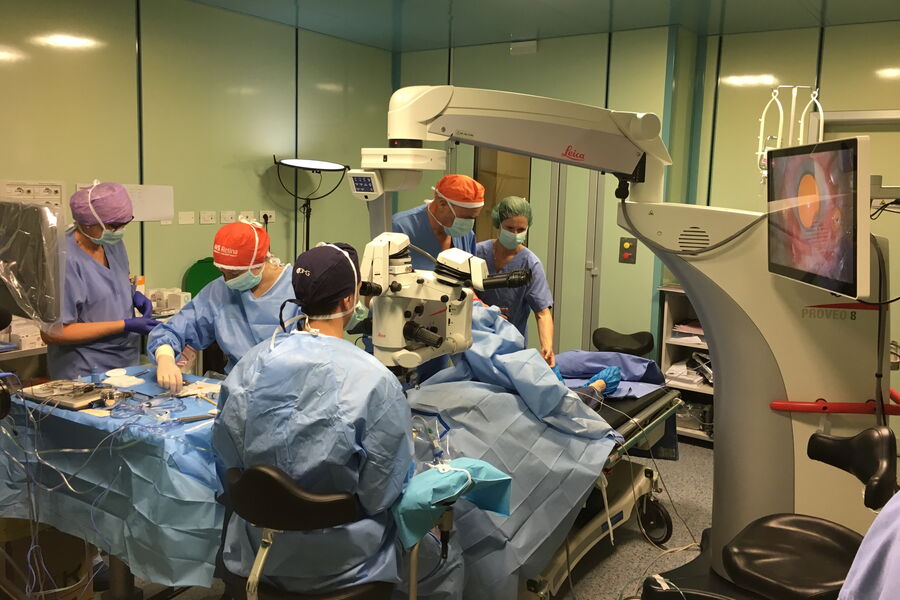
If the clinic seeks to move into teaching, integration of more extensive documentation or also teaching accessories such as viewing options for students can become relevant. Specifically for this purpose, 3D visualization technology becomes more and more frequent. Operating “heads-up” does away with the need for binoculars and enables teaching of nurses via screen. It’s worth checking whether an ophthalmic microscope can be used with a 3D visualization system. The M822 and the Proveo 8 ophthalmic microscopes by Leica Microsystems, for example, can be used with the NGENUITY® 3D Visualization System from Alcon, so that teaching takes on a new dimension.
Conclusion
Selecting an ophthalmic microscope for cataract procedures is no small feat. Before looking at the different makes and models on offer, the context in which the new tool is used should be described as accurately as possible. After this, talking to manufacturer representatives and looking at or even working with the microscopes is crucial to recognizing differences and honing the description of what is really needed. This will give surgeons a sound basis for their decision.