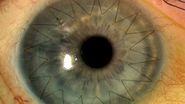
A macular hole is a rare eye condition that blurs central vision and impacts everyday tasks. Macular holes are usually caused by stretching or pulling the macula, causing an opening to occur. Typically, the most common cause of macular holes is age-related changes to the eye. However, in this case study Robert A. Sisk , MD, FACS presents a pediatric ophthalmology case in which intraoperative optical coherence tomography provided him with additional insights during surgery.
Watch the clinical video
This clinical case video was recorded during the 2022 Leica in Scope – Ophthalmology Visualization Summit webinar series event. The statements of the healthcare professional included in this video reflect only their opinions and personal experiences and not those of Leica Microsystems. They also do not necessarily reflect the opinions of any institution with which they are affiliated. Please note that off-label uses of products may be discussed. Please check with regulatory affairs for cleared indications for use in your region.
Case Description
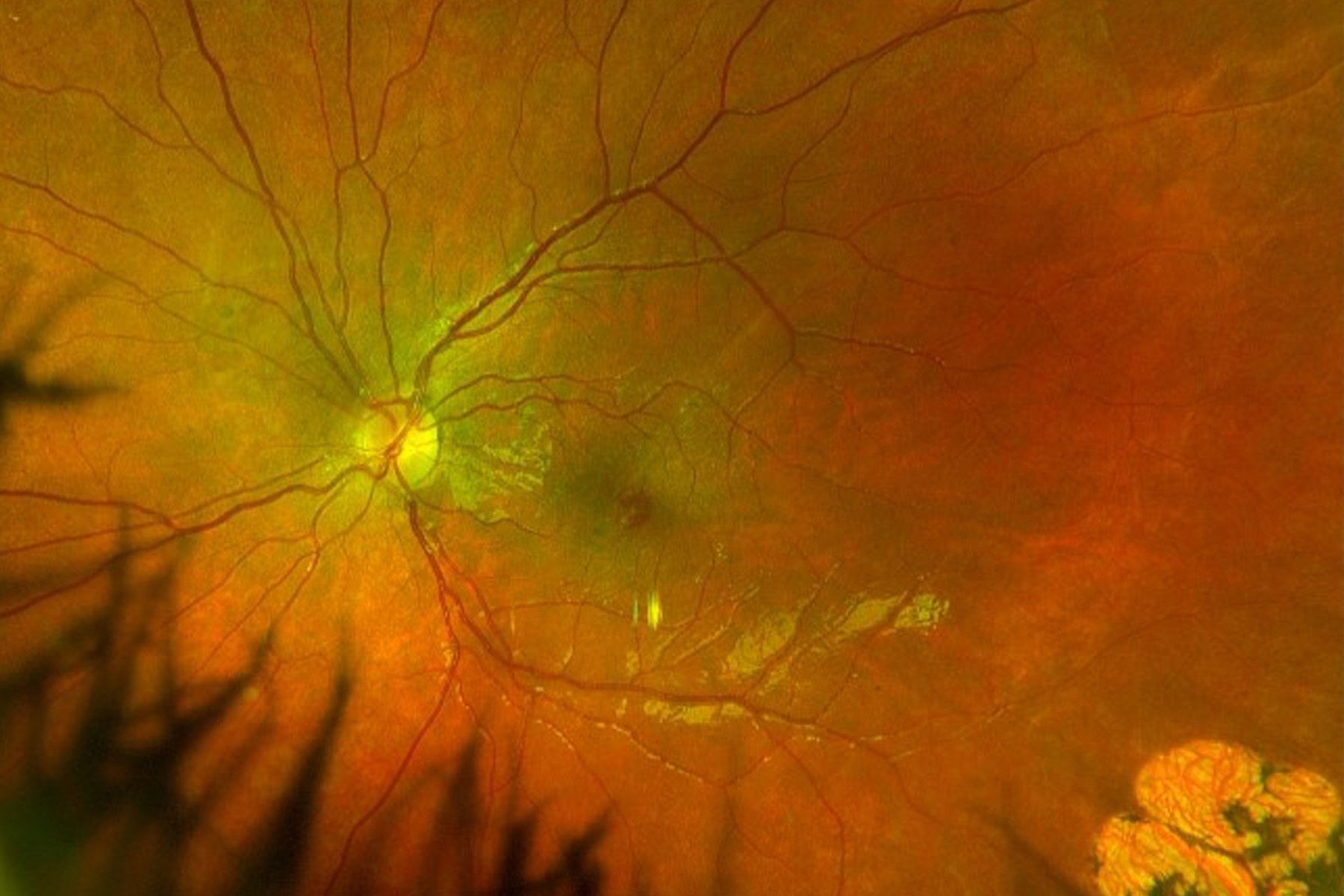
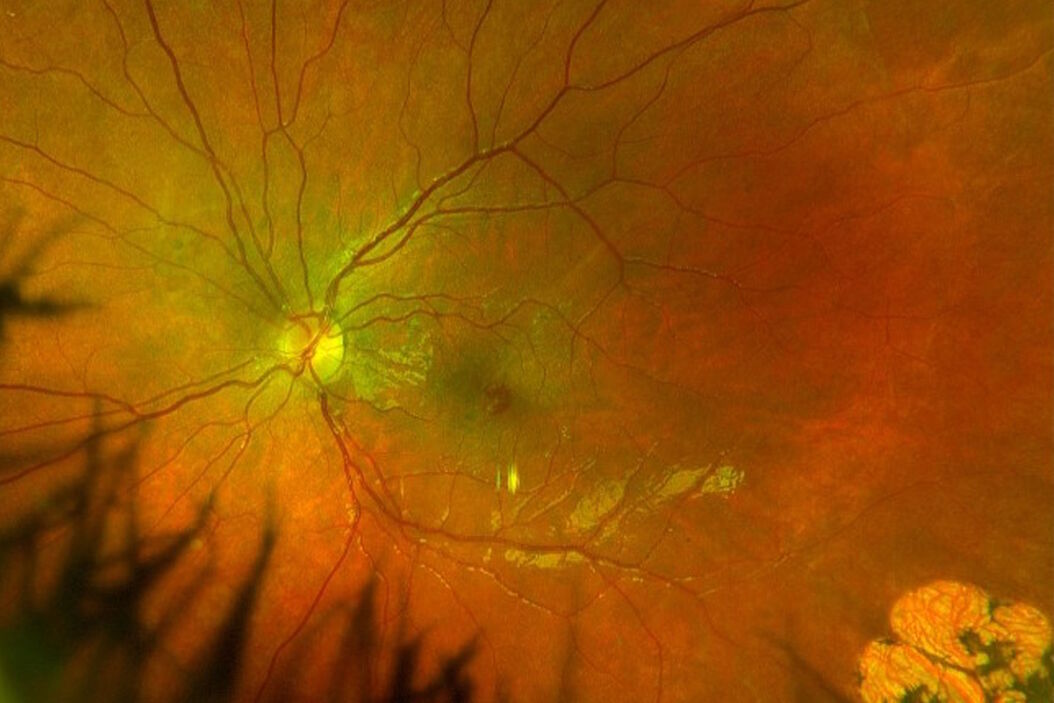
A 9-year-old boy presented with complaints of blurred and distorted vision in the left eye. He had congenital cystic encephalomalacia that resulted in seizures and multiple falls in his early childhood. There was no recent trauma or family history of seizure disorder, and he was neurologically intact.
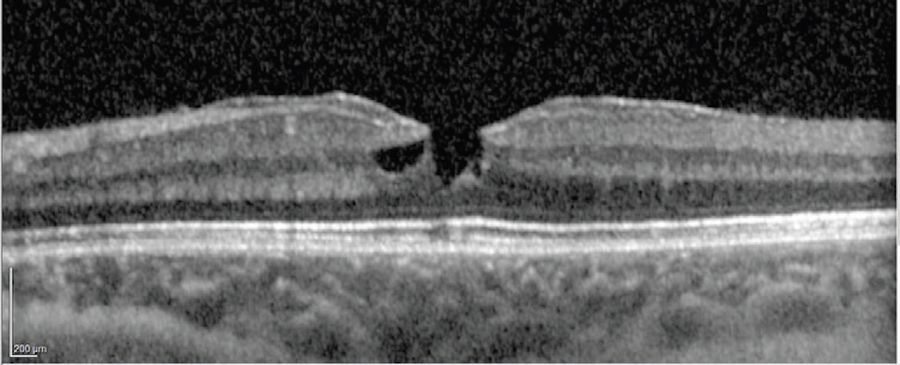
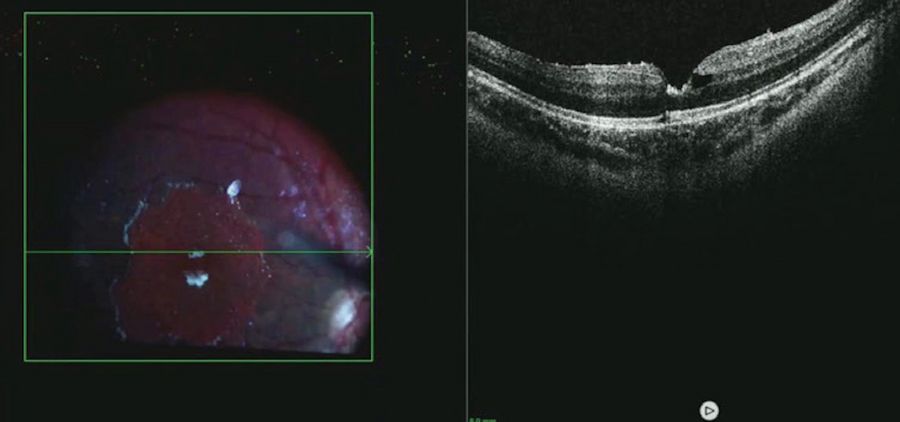
On examination, the anterior segment was normal but both eyes had an epiretinal membrane, greater in the left eye, with lamellar macular hole.
There was no hearing loss or family history of neurofibromatosis type 2. The boy was having difficulty playing sports due to reduced depth perception, especially with baseball.
Pre-operative assessment
Visual acuities were subnormal in both eyes, and particularly in the left eye at 20/60. There was an area of chorioretinal scarring temporally in the left eye. This may represent resolution of previous commotio retinae.
Surgical approach
The surgical plan was to remove the epiretinal membrane, elevate the epiretinal proliferation and use an ILM flap to close the lamellar macular hole.
Vitrectomy was performed. The hyaloid face was still attached to the optic nerve, as expected for a 9-year-old boy. There was some mild vitreous condensation and partial vitreous separation superotemporally.
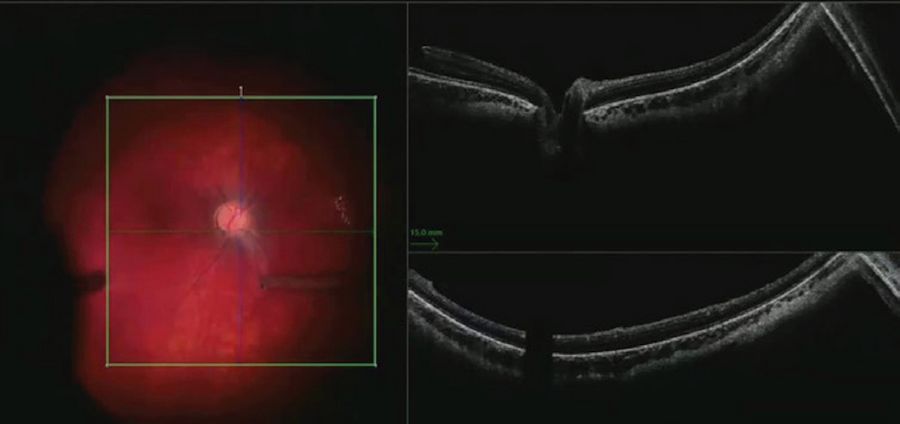
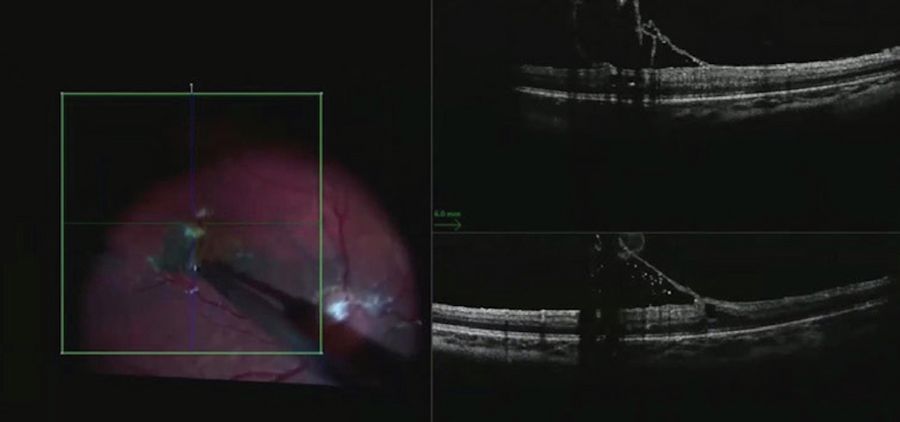
The hyaloid face was elevated by aspiration from the optic disc. The intraoperative OCT was helpful to see where the hyaloid was still attached during these maneuvers (Figure 2). In the case of split or tenacious hyaloid, triamcinolone stain can be helpful to visualize the vitreous both under the microscope and on the live intraoperative OCT images.
The hyaloid was then peeled from the area of adherence by aspiration. After the vitreous membranes were removed, heavy ICG was used to stain the ILM and counterstain the epiretinal membrane.
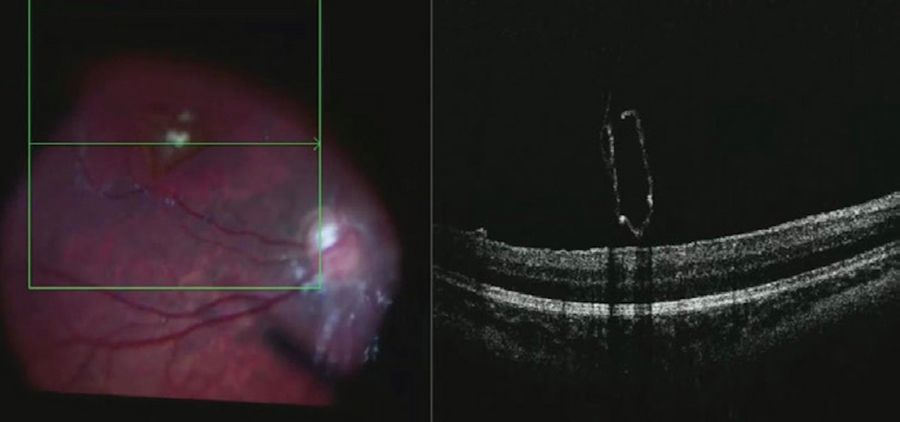
Intraoperative OCT provided valuable real-time insights on the configuration of the membrane, which can change after the hyaloid is lifted (Figure 3).
With a nitinol loop, an inferior ILM flap was created to peel the epiretinal membrane and ILM together. A wide flap allowed more room to peel circumferentially around the fovea without placing excessive traction on the fovea.
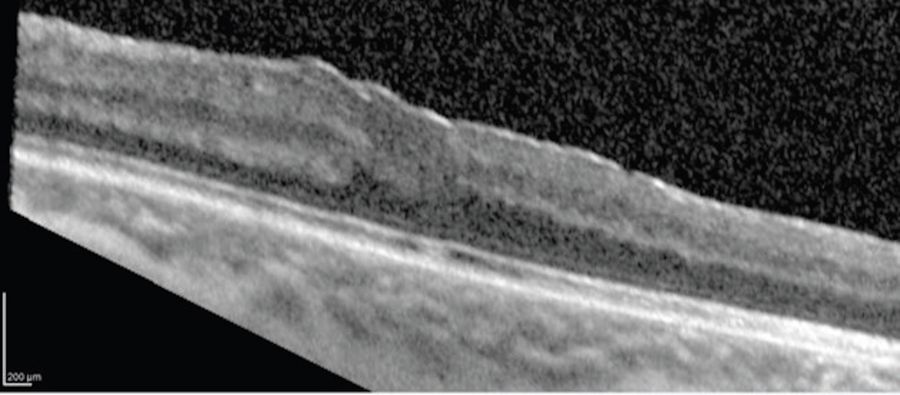
As the membrane was peeled up to the fovea, the intraoperative OCT showed the surgeon when to stop pulling to avoid amputating the epiretinal proliferation. This is critical as the visual cues are not always optimal during this type of maneuver (Figure 4).
The cabbage leaf plume of epiretinal tissue was elevated and then trimmed with the vitreous cutter on shave mode. The surgeon was careful to avoid removing tissue stained yellow by luteal pigments as the goal was to preserve the tissue for reintegration into the fovea. A final scan was performed to confirm traction was removed from the edges of the lamellar hole before the fluid air exchange (Figure 5).
The patient was positioned face down during the first day after surgery.
Post-operative outcomes
One month post-operatively, the patient had reduced distortion and improved real-world function. He also had improved depth perception and color vision and was able to see the ball better during sports. Further improvement was expected with longer follow-up (Figure 6).
Conclusions
Intraoperative OCT provided valuable insights during macular hole repair that differ from preoperative OCT scans. When the hyaloid face is thick, the configuration of the epiretinal membrane may change after the hyaloid face is elevated. Also, surgical planes may open intraoperatively that can be exploited for membrane peeling- these may not be present in the pre-operative OCT. Biological stains such as triamcinolone can adhere to the hyaloid or epiretinal membrane and provide additional registration points for finding the posterior hyaloid on the live intraoperative OCT.
In addition, intraoperative OCT supports reintegrating the ectopic foveal tissue into the lamellar MH repair. Inverted flaps are notorious for dislocating, but this depends upon the adherence of the ILM or epiretinal membrane at the margins of the macular hole. The intraoperative OCT scan can help the surgeon identify the limits for peeling, show whether the ILM flap amputated, or confirm that a free flap remains in place with the final tamponade. These features can provide a better anatomic and functional outcome for these challenging cases.
The statements of the healthcare professional included in this case study reflect only their opinions and personal experiences and not those of Leica Microsystems. They also do not necessarily reflect the opinions of any institution with which they are affiliated. Please note that off-label uses of products may be discussed. Please check with regulatory affairs for cleared indications for use in your region.