Watch the clinical video case now
This clinical case video is from the 2022 Leica in Scope – Ophthalmology Visualization Summit webinar series event.
The statements of the healthcare professionals included in this clinical case video reflect only their opinions and personal experiences and not those of Microsystems. They also do not necessarily reflect the opinions of any institution with which they are affiliated. Please note that off-label uses of products may be discussed. Please check with regulatory affairs for cleared indications for use in your region.
First Clinical Case: Thin Manual Descemet Stripping Endothelial Keratoplasty (TM-DSEK)
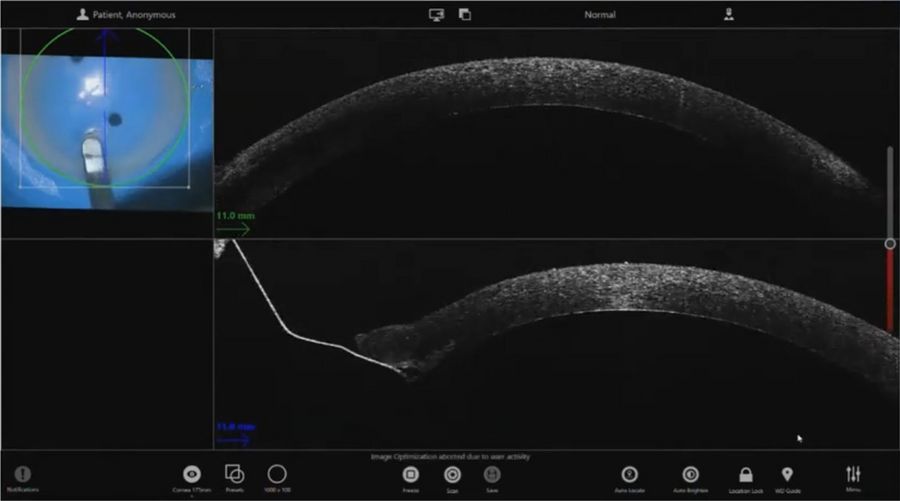
In this case, a Descemet rhexis was created. The clear red reflex on the Proveo 8 with EnFocus intraoperative OCT allowed clear visualization of Descemet’s membrane peeling and endothelium.
When performing DSEK in eyes that have had a penetrating keratoplasty or other pathologies such as posterior membrane dystrophies, it is valuable to see DM as opposed to stromal tears or folds.
In TM-DSEK, it is possible to leave some of the DM present whereas in DMEK, DM is stripped beyond the border of the graft.
When performing the strip, the intraoperative OCT provided live confirmation of where DM was present. This is particularly helpful when there is a poor view e.g. in this case of ocular trauma. The OCT showed the separation of Descemet’s membrane very clearly.
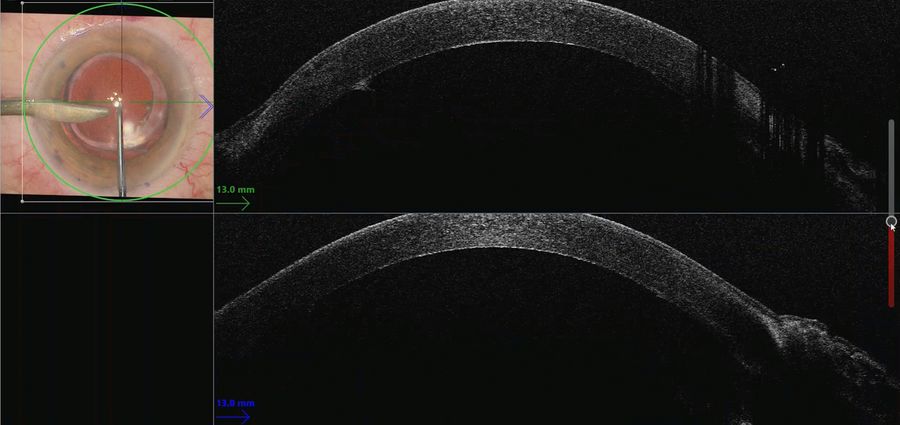
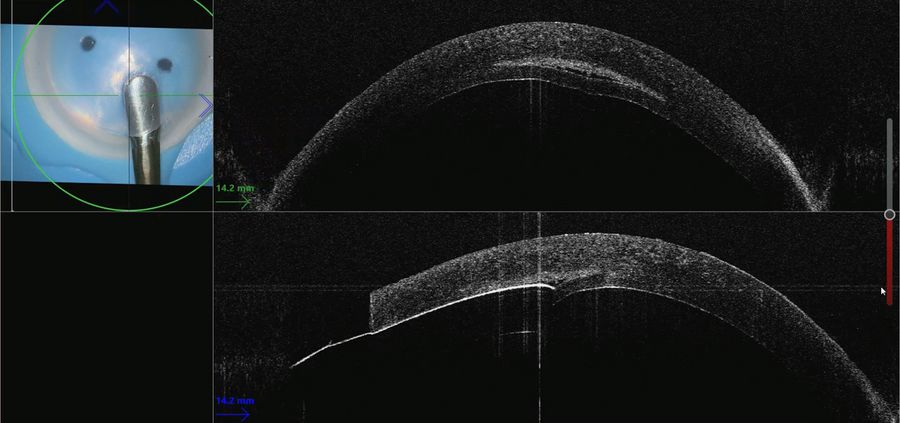
In the first stage of the dissection, a preset depth cut was performed with the diamond blade preset to a depth of 550 microns. The intraoperative Optical Coherence Tomography helped accurately assess progression. Based on this assessment, the cut can be made safely with increasing depth as needed. This is important as all corneas are different, and it can be difficult to know the depth of the cornea before making the incision. This helps by avoiding perforation of the cornea at this stage.
After making an accurate depth incision, dissection was performed with a Paufique blade. The cornea-scleral rim was in an artificial anterior chamber, which was full of air. This type of dissection is not easy to perform and there is a significant perforation risk when dissecting down. The surgeon needs to make the dissection to the required depth quite quickly because as the tip of the blade moves forward towards the center of the cornea, it is important for the center of the cornea to be as thin as possible avoiding a thick wedge dissection (where the beginning of the incision is quite thick and then thins progressively).
The intraoperative Optical Coherence Tomography allowed visualization in real-time which is a major benefit. As the surgeon made the dissection down, he could see the curved reflection at the tip of the blade. He could also stop the dissection at any stage during the surgery to look at where the tip of the blade was relative to the corneal endothelium. This allows dissection down to the correct level much faster and more safely.
A lamellar splitter was then used. The objective was to maintain the plane that had been originally defined. The lamellar splitter defined the plane going forward as the cornea was split. Dissecting forward across the midline, it was important to ensure the correct plane was maintained because all dissectors move in a straight line and would naturally result in the dissection becoming more shallow. The dissection should follow the curve of the cornea so that the endothelium disc is the same thickness all the way across.
At this stage, the dissection was nearly completed, going under the limbus to make sure that, when punching out the donor disc, there wouldn’t be any tags of tissue between the two layers. The intraoperative Optical Coherence Tomography was actively moved during the surgery to center the image as needed. The surgeon was very free with movements during the surgery and could move the artificial anterior chamber as well as his hands, always remaining in focus without the need to stop and realign the focus.
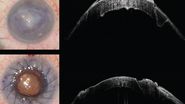
On one of the grafts that had been introduced, the intraoperative Optical Coherence Tomography showed two important aspects. On the upper surface of the donor lenticule, there was a ruffled superior edge, and the
stromal fibers were visible, which we have termed the ‘Sunspot Sign’ as they resemble the solar flares emanating from the Sun. The hyperlucent smooth reflective image at the bottom of the lenticule indicated the endothelium. As such, intraoperative Optical Coherence Tomography helped tell the difference between the two sides of the donor lenticule and ensure the correct orientation of the tissue.
Clinical Case 2: Big-Bubble Deep Anterior Lamellar Keratoplasty (DALK)
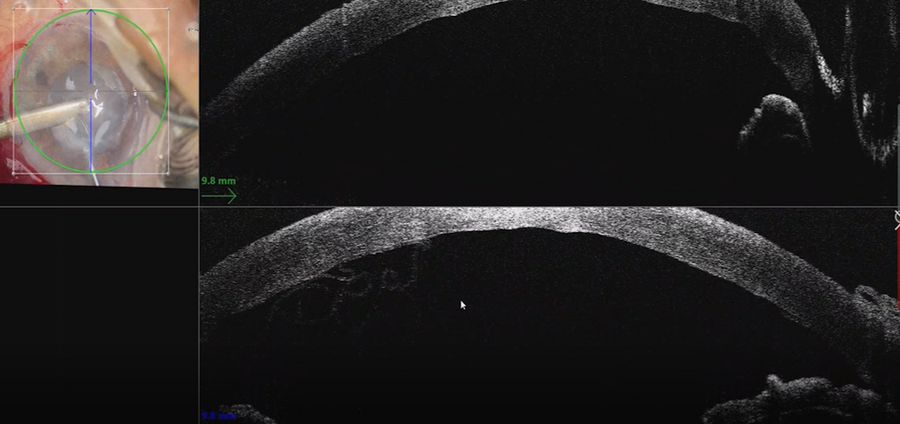
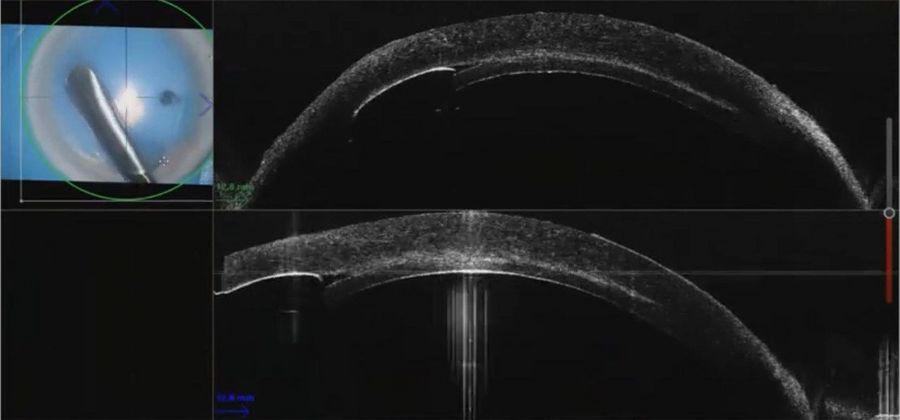
This is a procedure that can be tricky to learn, even for experienced corneal surgeons. In this case of Keratoconus, the cornea was typically thin. The trephine was rotated to cut down 200 microns and the canula was then introduced at the depth of the trephination. The intraoperative Optical Coherence Tomography helped inform the positioning of the canula in the cornea, showing it was above the PDL (pre-Descemet layer) and that there was some tissue between the PDL and DM.
The anterior part of the cornea was removed. After the removal, a shiny surface was observed beneath it and air in the anterior chamber. A small bubble was visible between the dissector and the PDL indicating that the
dissection had not quite reached PDL. Further dissection in this situation risks perforating PDL so visualization of this space is an important aid to avoid perforation of DM whilst dissecting as close to PDL as possible.
The images showed the instrument was underneath tissue and above the PDL. This information could only be obtained through intraoperative Optical Coherence Tomography.
Clinical Case 3: Descemet Membrane Endothelial Keratoplasty (DMEK)
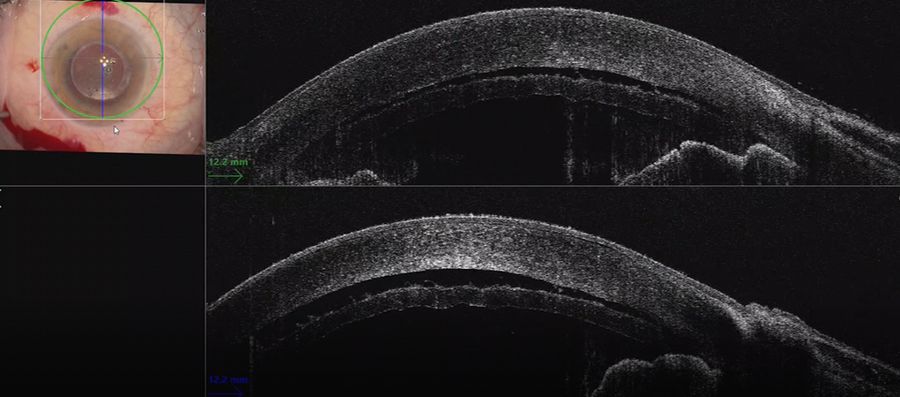
In this case of DMEK, intraoperative Optical Coherence Tomography showed the DMEK scroll being flattened out. As the cornea was massaged, fluid was gradually released from between the DMEK and the host stroma. Employing a 360° intraoperative Optical Coherence Tomography scan confirmed the attachment, with a more clearly defined edge to the DMEK graft in the microscope view and a clear view of the attachment through intraoperative Optical Coherence Tomography.
Conclusions
The use of Proveo 8 with EnFocus intraoperative Optical Coherence Tomography in endothelial keratoplasty supports optimal surgical outcomes and can increase the speed and safety of procedures.